Retrograde Tibio-Pedal Access for Revascularization of Lower-Extremity Peripheral Artery Disease Using a 6 Fr Slender Sheath: The "Pedal-First" Pilot Project
Abstract: Objective. We studied the safety and efficacy of tibio-pedal access (TPA) as the sole primary access (ie, the “pedal-first” strategy) for revascularization of peripheral artery disease (PAD). Methods. We reviewed a prospectively maintained database of patients where TPA was used as a primary access for retrograde diagnostic angiography and intervention. Patients suffering from symptomatic PAD and abnormal non-invasive testing were treated with the intention of using only ipsilateral TPA if there was antegrade flow in one of the three run-off vessels on ultrasound (US). Additional radial or femoral access (FA) was used only if needed for successful revascularization. TPA was achieved with US guidance using a 6 Fr thin-walled hydrophilic sheath. Patency of the accessed tibio-pedal artery was evaluated with US at 30 days. Results. The pedal-first approach was attempted for 41 limbs in 36 patients. The overall rate of successful revascularization was 95% (39 limbs). TPA was successfully used in all 39 limbs and “pedal-only” success occurred in 30 limbs (77%). Two procedures were unsuccessful in revascularizing target-vessel occlusion despite dual access. Patients without FA were able to ambulate at an average of 3 hours post procedure. No acute vascular access-related complications were noted. Each accessed tibio-pedal artery was patent on US evaluation at 30 days. Conclusion. The pedal-first approach of using TPA with a 6 Fr thin-walled sheath as a primary access and as the only access for diagnosis and intervention of PAD is safe and highly successful in carefully selected patients.
J INVASIVE CARDIOL 2018;30(9):334-340.
Key words: endovascular intervention, peripheral artery disease, tibial-pedal artery access, vascular access
Endovascular revascularization of symptomatic lower-extremity peripheral artery disease (LEPAD) has advanced dramatically over last 15 years due to improved understanding of the disease process and development of effective treatment technologies and techniques.1 One of the major technical evolutions has been the hybrid approach with antegrade and retrograde access.2-8 Tibio-pedal access (TPA) for revascularizing critical PAD is safe and increases the procedural success rate in patients with critical limb ischemia (CLI).2-8 TPA has mainly been used as a secondary access to cross through occlusions while using femoral access (FA) as the primary access. While all the reports to date support safe use of 4 Fr sheaths and 4-Fr compatible devices through TPA,2-8 it remains unknown if the use of a larger introducer that allows the use of contemporary interventional therapy is safe for TPA.
The 6 Fr thin-walled arterial access sheath (Terumo Corporation) has the inner diameter of a 6 Fr sheath with the approximate outer diameter of a 5 Fr sheath (~2.45 mm) to keep the arteriotomy size smaller while allowing passage of larger-caliber equipment. After achieving experience with TPA, in April 2015, we started what we called the “pedal-first” approach for carefully selected patients. The intention was to use TPA as the primary access as well as the only access for diagnostic angiography and intervention of ipsilateral leg symptomatic PAD. The goal of the pedal first approach was to prevent potential vascular complications associated with FA, allow immediate sitting up, early ambulation and discharge, as well as to hopefully improve the cost of the procedure while still offering the most contemporary evidence-based treatment of LEPAD.
The primary objective of this single-center retrospective analysis of prospectively maintained data was to study success rate, safety, and efficacy of TPA as the primary access (pedal first) and as the only access (pedal only) for revascularization of LEPAD.
Methods
Study design. This is a single-center prospective review of a database of patients who underwent endovascular intervention of their PAD with attempted pedal first approach by a single operator. The cath lab database was queried to identify patients who underwent endovascular intervention of LEPAD and received TPA since 2015. The patients were then selected if the TPA was attempted as the primary access or first access with the intention to use TPA as the only access. Patients in whom either radial access (RA) or FA was obtained first or used as primary access were excluded. Demographic data, clinical history, clinical presentation, procedural data, and postprocedure data were collected by retrospective review of prospectively maintained electronic medical records. Approval by the institutional review board was obtained prior to conducting the study.
Patient and access-vessel selection. Patients with symptomatic PAD (Rutherford class 2-5) despite optimal medical management and who had significantly abnormal ankle-brachial index (ABI)/pulse-volume ratio (PVR) were brought to the catheterization suite for endovascular intervention of the LEPAD. Based on clinical history, ABI/PVR, and duplex sonography, the patients with high likelihood of primary femoro-popliteal disease were selected for pedal-first approach. Patients with a high likelihood of only in-flow disease were avoided. A primary operator performed an ultrasound evaluation of the outflow vessels near the ankle joint in the preprocedure area. The pedal-first approach was attempted if there was antegrade flow in one of the three run-off vessels at or near the ankle, and if the artery appeared to be healthy for access based on the operator’s experience. This preprocedure ultrasound (US) evaluation was used to guide the selection of the tibio-pedal artery site for access and the skin was marked with a marker pen. The patient was then placed on the cath lab table in a supine position. The radial area and groin were prepped as required for possible secondary access.
Method for access. The entire ipsilateral leg (lower half of thighs to the toes) with the target PAD was prepped and draped with standard antiseptic and aseptic precautions, exposing the drape at the planned access site. If the patient could cooperate for posterior tibial (PT) access, he or she was asked to have slight flexion at the knee and external rotation at the hip to allow easier ergonomics for the operator. For anterior tibial (AT) and peroneal access, supine position of the foot with some plantar flexion was preferred if the patient could do so comfortably. A hockey stick probe and vascular US with the Zonare Zone Ultra system (Zonare Medical) were used to guide the advancement of the needle. One of the three arteries per operator choice was accessed with a 21 gauge Jelco AngioCath (Smiths Medical) using a posterior-wall (double-wall) puncture technique.9 After removing the needle, the Teflon cannula of the AngioCath was slowly withdrawn parallel to the course of the artery until arterial flow was seen. A 0.021˝ access wire or 0.014˝ coronary wire was inserted carefully under fluoroscopic or US guidance. In patients with severe abnormal outflow on the ABI or when the posterior-puncture technique failed, a 21 gauge micropuncture needle was used for anterior-wall puncture technique. A skin incision was created to facilitate sheath entry. A 6 Fr thin-walled “slender” sheath was inserted over the wire, holding the sheath with a wet towel to activate hydrophilic coating (Figure 1). An antispasmodic cocktail of 200 µg nitroglycerin and 2.5 mg verapamil was injected through the sheath into the artery. Intravenous heparin (70 unit/kg) was given immediately with access and more heparin was given throughout the procedure as required to keep the activated clotting time (ACT) >250 seconds.

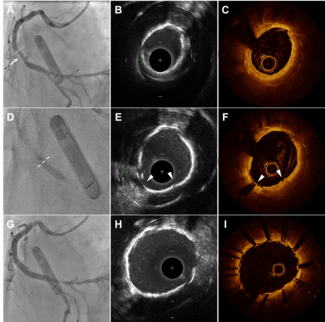
Method for performing procedure. Baseline arterial pressure was recorded through the sheath (Figure 2). Arterial angiography of the outflow circulation was performed using 50:50 diluted contrast and digital subtraction angiography (DSA) (Figure 3A). Guided by the angiography or image-overlay technique, a 0.014˝ workhorse wire, 0.018˝ V18 control wire (Boston Scientific), or 0.035˝ hydrophilic angled Glidewire (Terumo) was advanced through the sheath along with either a 0.018˝ or 0.035˝ Quick-Cross support catheter (Spectranetics) in retrograde fashion. Retrograde angiography of the popliteal artery and superficial femoral artery (SFA) was performed using the Quick-Cross in the popliteal artery (Figures 3B and 3C). Based on the anatomy and the nature of the lesion, either an 0.014˝ wire, 0.018˝ wire, chronic total occlusion (CTO) wire, or CTO crossing device were used at the operator’s discretion to cross the lesions in the popliteal/SFA/or common femoral artery (CFA) distributions. A crossing catheter was advanced over the wire retrograde through the crossed lesion into the CFA and/or iliac artery, and angiography was performed (Figures 3D and 3E). Proximal iliac artery or aortic pressures were recorded. When unable to cross through the occluded artery, or whenever antegrade angiography of the inflow was required, a secondary access was obtained. Left radial artery was chosen whenever possible or convenient; alternatively, the contralateral CFA was used (Figure 4). Irrespective of access choice, contemporary occlusion crossing strategies, including subintimal technique10,11 and SAFARI technique12 were used. Guided by the angiography and radiopaque ruler, disease segments were treated with different treatment modalities at operator’s discretion (Figure 5). Repeat angiography was performed by advancing a 0.035˝ crossing catheter or 4 Fr hydrophilic Glide catheter (Terumo). Between every device exchange, robust flushing of the pedal sheath was performed and pressures were recorded. After the intervention, a final angiography of the entire leg including the outflow was performed using DSA. Final pressure at the TPA from the sheath was recorded (Figure 2).




Method for hemostasis and postprocedure care. In patients with peroneal artery access, manual pressure was applied after removing the sheath immediately after completion of procedure. A Vasostat hemostatic band (Forge Medical) or a Safe Guard Radial band (Merit Medical) was used for hemostasis if AT or PT artery was accessed (Figures 6A, 6B, and 6C). After applying the band over the skin entry site, hemostatic pressure was applied by injecting air in the Safe Guard band or by pushing the plunger in the Vasostat band; the sheath was then removed. The pressure was reduced slowly to the point when the bleeding was seen, and then pressure was increased slightly to provide just enough pressure to achieved hemostasis. The access site was monitored for 5 minutes to confirm that the minimal pressure applied was maintaining the hemostasis. Every 30 minutes after the band application, the access site was checked post intervention by the ward nurse and pressure was reduced incrementally if there was no bleeding seen. The band was removed 1-2 hours after placement (no later than 2 hours) and an adhesive bandage was applied at the site. Radial artery hemostasis was achieved with a TR band (Terumo). Femoral artery hemostasis was achieved using a closure device or manual compression after the normalization of ACT at the operator’s discretion. Patients were discharged home at 4-6 hours post procedure if clinically stable without any complications (Figure 6D). Patients were followed up at 30 days post procedure with ABI/PVR of the target limb and US of the accessed tibial-pedal artery.

Results
Between April 2016 and April 2017, pedal access was attempted in 112 out of 506 LEPAD interventions at our cardiac cath lab. The pedal-first approach was attempted for treating 41 lower extremities in 36 patients during this period. The patients presented with Rutherford class 2-5 symptoms. Demographic, clinical presentation, and lesion characteristics are described in Table 1. TPA was achieved successfully in 39 limbs (access success rate, 95%). The TPA attempts were unsuccessful in 2 limbs; both were then treated with traditional contralateral femoral approach. US guidance was used during all 41 attempted TPA procedures (100% US use). Thirty-nine LEPAD patients were revascularized successfully (procedural success rate, 95%) with pedal-only success in 30 limbs (pedal-only success rate, 77%), requiring additional secondary (ancillary) access for successful revascularization in 9 limbs (4 RA and 5 FA). Two of the 39 successful TPA procedures were accessed prior to the study period, and both were successfully accessed again during the study period.

Two procedures were unsuccessful in revascularizing target-vessel occlusion despite dual access including pedal and femoral access. All but 1 patient requiring additional secondary access had a CTO of either the SFA, popliteal, or accessed tibial-pedal artery. Fifty-nine target-lesion segments in 39 limbs were revascularized successfully (Table 1). While most patients had primarily SFA/popliteal lesions due to patient selection methods, diseases in outflow as well as inflow vessels were revascularized successfully when required through pedal-only approach (Table 1). Different treatment modalities including directional atherectomy, LASER atherectomy, orbital atherectomy, balloons, drug-eluting balloons, and self-expanding stents were used for the diseases treated (Table 2). None of the patients had access-vessel or target-vessel perforation, accessed artery dissection, acute thrombosis, or no-flow. None of the patients with TPA had large hematoma, compartment syndrome, or required emergency vascular surgery consultation. One patient with TPA had swelling of the leg, which was evaluated with computed tomography scan. The patient was found to have small hematoma on the scan and was managed conservatively with extended compression and observation without any further sequels (Figure 6C). Four patients with TPA complained of minor pain at the primary access site at the time of discharge. One patient with FA had large hematoma requiring transfusion and 1 patient with FA had small pseudoaneurysm managed with manual pressure. All patients without FA were able to sit up immediately, ambulated sooner, and had early discharge in comparison with those patients requiring FA as secondary access (Table 2). At 30-day follow-up, a total of 32 patients (88%) had clinical success, with improved symptomatology/Rutherford class and improvement in ABI/PVR from the baseline, while 1 patient had target-lesion revascularization for SFA stent thrombosis. One of the 2 patients with unsuccessful revascularization underwent planned vascular bypass surgery, while the other patient had repeat endovascular procedure that was successful for revascularization. At 30-day US evaluation, all 39 tibio-pedal arteries accessed were patent with antegrade flow. Furthermore, there were no adverse bleeding events noted at 30-day follow-up (Table 2).

Discussion
Despite advances in endovascular interventions, the most common complications of these procedures are related to vascular access.2 Vascular access-related complications are more frequent during diagnostic or interventional endovascular procedures in the presence of PAD.13-15 In the quest for improving vascular access complication rates, RA has been reported as an alternate access in registries and observational studies, with major limitations in equipment choices, sizes, and lengths due to the radial diameter and distance from the LEPAD.14-17
The tibio-pedal approach was initially used to promote limb salvage in critical limb ischemia (CLI) patients.2,3,6-8,18 Increasing expertise, improved tools, and low reported complication rates2-9 have led some institutions to permit a more liberal use of the tibio-pedal approach.5 Because of the superficial location and easy US penetration, US-guided TPA can be achieved with higher success and allows for easy compressibility and hemostasis. The shorter distance to the target lesion in the ipsilateral limb and straighter course improve the maneuverability of devices and torque transmission of wires. Efficient use of diluted contrast for the selective retrograde angiography and use of US can improve overall contrast and radiation utilization. Particularly for CTO revascularization, a retrograde approach has more success as the wire torque transmission is better, forward-force transmission is better, and the distal cap crossing is easier to cross than the calcified proximal cap.2-9 Furthermore, TPA allows easy supine positioning of the patient on the cath lab table and easy equipment parking. TPA also prevents the operator from reaching over the x-ray field, as occurs during a contralateral FA or left RA. In contrast to a FA procedure, a patient undergoing TPA can be propped up to 45° and sit up immediately after the procedure. Patients suffering from clinical conditions that prevent prolonged supine positioning, such as congestive heart failure, chronic obstructive pulmonary disease, sleep apnea, prostate enlargement, and spinal and other orthopedic conditions, are more likely to benefit from TPA. In patients who are at high risk for FA, such as those with morbid obesity, large pannus, or a severe calcified femoral artery, TPA could be another alternative. Similarly, in patients with severe aorto-iliac tortuosity, occlusion, or calcified disease with difficult or impossible anatomy for an up-and-over approach from the contralateral FA, TPA could be another alternative. Using TPA can avoid life-threatening complications, such as retroperitoneal bleed or large groin bleed requiring blood transfusions, and avoid FA pseudoaneurysm, which is a relatively common complication with a calcified FA. TPA (along with FA or RA) allows the “hybrid approach” and use of contemporary CTO revascularization devices and techniques, such as retrograde or antegrade dissection and re-entry, double-balloon technique,18 or SAFARI technique,12 and thus increases the technical and clinical success of the procedure. The retrograde pedal approach allows precise deployment of a self-expanding stent when ostial SFA stenting is required, as demonstrated in Figure 5.
With all of these advantages described, there is certainly a concern of injury or thrombotic occlusion of a pedal vessel that could either sacrifice a distal bypass target or lead to gangrene and amputation. This could convert a life-style issue to a limb-threatening issue. While treating complex infrapopliteal lesions, Montero et al reported 1 out of the 51 limbs with TPA had access vessel occlusion. Despite the tibio-pedal occlusion rate being very low,2-9 authors in the past3 strongly opted to reserve TPA only for CLI interventions, calling TPA an “extreme revascularization technique.” More recent use of a retrograde TPA is reported as a primary treatment for patients who are poor candidates for antegrade access6 or for the treatment of PAD patients suffering from claudication (Rutherford class 2-3) that has not yet progressed to CLI (Rutherford class 4-6).4-6,8 These recent reports4-6,8 showed high success and safety of TPA using a 4 Fr access and 4-Fr compatible intervention devices. Use of a 4 Fr introducer does not allow TPA to be the only or primary access, as contemporary evidence-based treatment of the LEPAD requires the use of a 6 Fr sheath in the majority of cases. Primary and secondary patency of PAD revascularization can be improved with adequate debulking of the plaque or calcium with appropriate-diameter atherectomy devices,20,21 drug-eluting balloons,21,22 self-expanding stents,23 and LASER atherectomy for in-stent restenosis,19 all of which require a 6 Fr introducer. Therefore, if TPA is to be used as the primary and only access, it will require a 6 Fr introducer to achieve higher clinical success rates and long-term patency. With a large institutional experience of TPA and a sizable safety experience of using a 6 Fr slender sheath for ancillary TPA, we were inspired to push the envelope and explore the safety, efficacy, and advantages of the pedal-first approach. Meticulous case selection, procedural care, and postprocedure evaluations were required while investigating this novel approach. Similarly, during this investigation, the fear of potential TPA occlusion and limb loss was real but was neutralized with the knowledge of FA-related complications including retroperitoneal bleeding and even fatalities reported in the literature.13-15 Preprocedure CT angiography of the lower extremities might have improved the patient selection process while investigating this novel approach, but was not used because of institutional limitations.
Although the data were evaluated retrospectively, we prospectively maintained the same procedure methods and recorded important safety endpoints. Hemodynamic evaluation of the TPA vessel at the time of access and at the end of the procedure confirmed the improved perfusion of the leg and ruled out no-flow. We did not encounter any acute or late thrombotic occlusion of the accessed tibio-pedal artery, but we were very careful in using meticulous aspiration and flushing techniques, administering aggressive anticoagulation, and achieving hemostasis with the least amount of pressure for the shortest duration of time. We did not encounter any dissection of the accessed tibio-pedal vessel despite using 6 Fr thin-walled sheaths on the final angiography evaluation of the outflow, which was performed in every case; however, angiography of the outflow vessel through the sheath is limited in evaluating flow distal to the access. Therefore, clinical evaluation of any skin color changes and pain at or distal to the access site were recorded prior to discharge. At 30 days post procedure, evaluation of the accessed vessel with US as well as ABI/PVR of the target limb were performed. None of the 39 accessed tibio-pedal arteries had occlusions at 30-day US evaluation; this is an encouraging result, especially when considered along with the advantages discussed earlier. The pedal-first and pedal-only approach requires further evaluation in multioperator, multicenter investigations; similar to RA, it may reduce discomfort, vascular access complications, morbidity, and mortality related to FA while allowing early ambulation, early discharge, and cost savings.
Study limitations. This is a single-center, single-operator, case series with clear selection bias, as the patients were carefully selected to evaluate this new pedal-first and pedal-only technique using a 6 Fr thin-walled sheath for TPA. The findings may not be applicable to all cath labs or operators due to lack of experience with pedal access. The sample size of this study is relatively small and does not reflect those patients who had TPA attempted as secondary or ancillary access during the same period. Despite no clinical complications, it is very difficult to visualize the distal artery beyond the access point and one cannot rule out the possibility of asymptomatic distal embolization. The current study findings cannot comment on any comparison with other vascular approaches; this would be useful information that requires a carefully planned future study. Nearly 1/4 of our study population required additional vascular access for successful revascularization, which is a limitation of the pedal-only approach.
Conclusion
The pedal-first technique of using TPA as a primary access and as the only access (pedal only) is feasible, highly successful, and safe in carefully selected patient cohorts. Being prepared to use either RA or FA as ancillary or secondary access allows contemporary techniques and technology for high procedural and clinical success in patients presenting with Rutherford class 2-5 symptoms. Use of TPA only or in combination with RA allows for immediate sitting up, early ambulation, and discharge. The use of a 6 Fr slender sheath allows operators to still use all of the contemporary intervention devices and current best practices for revascularization of PAD at multiple levels. Despite previous strong opinions against using 6 Fr TPA in non-CLI patients, at least in this cohort of carefully selected patients presenting with Rutherford class 2-5 symptoms, TPA with 6 Fr slender sheath access was safe. Further exploration of this novel pedal-first technique in comparative multicenter studies may help this minimally invasive, patient-friendly strategy gain popularity and give us another tool to help our patients who suffer from PAD.
References
1. Hong M, Beck A, Nelson P. Emerging national trends in the management and outcomes of lower extremity peripheral arterial disease. Ann Vasc Surg. 2011;25:44-54.
2. Mustapha JA, Saab F, McGoff T, et al. Tibio-pedal arterial minimally invasive retrograde revascularization in patients with advanced peripheral vascular disease: the TAMI technique original case series. Catheter Cardiovasc Interv. 2014;83:987-994.
3. Hernan A, Bazan LL, Donovan M, et al. Retrograde pedal access for patients with critical limb ischemia J Vasc Surg. 2014;60:375-382.
4. Kwan T, Shah S, Amoroso N, et al. Feasibility and safety of routine transpedal arterial access for treatment of peripheral artery disease. J Invasive Cardiol. 2015;27:327-330.
5. Walker CM, Mustapha JA, Zeller T, et al. Tibiopedal access for crossing of infrainguinal artery occlusion. J Endovasc Ther. 2017;23:839-846.
6. Hanna EB, Prout DL. Combined radial-pedal access strategy and radial-pedal rendezvous in the revascularization of complex total occlusions of the superficial femoral artery (the “no femoral access” strategy). J Endovasc Ther. 2016;23:321-329.
7. Montero-Baker M, Schmidt A, Bräunlich S, et al. The retrograde approach for BTK chronic total occlusions. Endovascular Today. 2014;5:55-64.
8. Walker C. Pedal access in critical limb ischemia. J Cardiovasc Surg (Torino). 2014;55:225-227.
9. Pancholy S, Sanghvi K, Patel T. Radial artery access technique evaluation trial: randomized comparison of Seldinger versus modified Seldinger technique for arterial access for transradial catheterization. Catheter Cardiovasc Interv. 2012;80:288-291.
10. Nasim A, Sayers RD, Bell PR, Bolia A. Recanalization of the native artery following failure of a bypass graft. Eur J Vasc Endovasc Surg. 1995;10:125-127.
11. Yilmaz S, Sindel T, Ceken K, Alimoğlu, Lüleci E. Subintimal recanalization of long superficial femoral artery occlusions through the retrograde popliteal approach. Cardiovasc Intervent Radiol. 2001;24:154-160.
12. Spinosa DJ, Harthun NL, Bissonette EA, et al. Subintimal arterial flossing with antegrade-retrograde intervention (SAFARI) for subintimal recanalization to treat chronic critical limb ischemia. J Vasc Interv Radiol. 2005;16:37-44.
13. Samal AK, White CJ. Percutaneous management of access site complications. Catheter Cardiovasc Interv. 2002;57:12-23.
14. De Belder AJ, Smith RE, Wainwright RJ, et al. Transradial artery coronary angiography and intervention in patients with severe peripheral vascular disease. Clin Radiol. 1997;52:115-118.
15. Trani C, Tommasino A, Burzotta F. Pushing the limits forward: transradial superficial femoral artery stenting. Catheter Cardiovasc Interv. 2010;76:1065-1071.
16. Sanghvi K, Kurian D, Coppola J. Transradial intervention of iliac and superficial femoral artery disease is feasible. J Interv Cardiol. 2008;21:385-387.
17. Staniloae C, Korabathina R, Yu J, et al. Safety and efficacy of transradial aortoiliac interventions. Catheter Cardiovasc Interv. 2010;75:659-662.
18. Schimidt A, Bausback Y, Piorkowski M, et al. Retrograde recanalization technique for use after failed antegrade angioplasty in chronic femoral artery occlusion. J Endovasc Ther. 2012;19:23-29.
19. Dippel EJ, Makam P, Kovach R, et al. Randomized controlled study of excimer laser atherectomy for treatment of femoropopliteal in-stent restenosis: initial results from the EXCITE ISR trial (EXCImer Laser Randomized Controlled Study for Treatment of FemoropopliTEal In-Stent Restenosis). JACC Cardiovasc Interv. 2015;8:92-101.
20. Ramaiah V, Gammon R, Kiesz S, et al. Midterm outcomes from the TALON registry: treating peripherals with SilverHawk—outcomes collection. J Endovasc Ther. 2006;13:592-602.
21. Cioppa A, Stabile E, Popusoi G, et al. Combined treatment of heavy calcified femoro-popliteal lesions using directional atherectomy and a paclitaxel coated balloon: 1-year single centre clinical results. Cardiovasc Revasc Med. 2012;13:219-223.
22. Laird J, Schneider P, Tepe G, et al. Durability of treatment effect using a drug-coated balloon for femoropopliteal lesions. J Am Coll Cardiol. 2015;66:2329-2338.
23. Katsanos K, Spiliopoulos S, Karunanithy N, Krokidis M, Sabharwal T, Taylor P. Bayesian network meta-analysis of nitinol stents, covered stents, drug-eluting stents, and drug-coated balloons in the femoropopliteal artery. J Vasc Surg. 2014;59:1123-1133.
From the Department of Interventional Cardiology, Deborah Heart & Lung Center, Browns Mills, New Jersey.
Disclosure: The authors have completed and returned the ICMJE Form for Disclosure of Potential Conflicts of Interest. Dr Sanghvi reports speaker honoraria from Terumo, Medtronic, Volcano, and Cordis Corporation; research grant (institutional) from Recor Corporation. The remaining authors report no conflicts of interest regarding the content herein.
Manuscript submitted July 16, 2018, provisional acceptance given July 19, 2018, final version accepted July 24, 2018.
Address for correspondence: Kintur Sanghvi, MD, FACC, FSCAI, Deborah Heart & Lung Center, 200 Trenton Road, Browns Mills, NJ 08015. Email: sanghvik@deborah.org