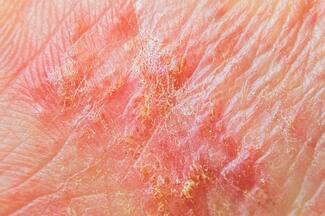
Treating Generalized Pustular Psoriasis
Generalized pustular psoriasis (GPP) is a rare but life-threatening condition that requires early recognition and prompt intervention. In this interview, Fabrizio Galimberti, MD, discusses how to differentiate GPP from other forms of psoriasis, the role of IL-36 in disease pathogenesis, and the latest advancements in targeted therapies. Learn practical strategies for managing flares, optimizing treatment, and improving outcomes for patients with this complex dermatologic condition.
Dr Galimberti is board certified in dermatology and micrographic dermatologic surgery by the American Board of Dermatology in Conway, SC.
Transcript:
GPP is a distinct autoinflammatory disorder with systemic complications. How should dermatologists differentiate GPP from other forms of psoriasis in clinical practice, and what are the key diagnostic red flags?
So, incredibly important question. So, it is a rare, chronic, and life-threatening conditions. So it's important to recognize it even though you might not see it every day. So first of all, the rapid onset is crucial. A lot of these patients will go from clear skin to really having a severe rash that covers most of their body relatively quickly, and that's a little bit different from the plaque psoriasis that we usually think of. They will have pustules and erythema, so they're going to be red, they're going to have all these pustules, something that we usually don't see in plaque psoriasis, even though they might have a background of plaque psoriasis. But importantly, they're going to have some systemic symptoms, fever, chills, malaise. You're going to find some inflammation in their body with the level of CRP and ESR. So, there's going to be some systemic findings lab wise, but also when you talk to the patients, interestingly enough, of course these postures are sterile, so they're not infected.
There's not nothing if you grow them, if you try to culture them, but interestingly enough, you might find something there because infections can trigger that. And very importantly, this is a life-threatening condition potentially. So a lot of these patients, even though in dermatology, we don't think of hospital admissions very often, direct hospital admissions if we suspect GPP, and we're able to identify and diagnose, and that's why this is important, that we might need to even send in directly to the emergency room if we work in the hospital directly. Now, there are some parameters in diagnosing GPP, particularly the Japanese Dermatology Association has come up with a list of criteria. They're relatively easy to just identify by looking at the patients. So that's why I love them and asking the question. So you must have systemic symptoms, fatigue, fever, fatigue. So the patient must feel a little bit under the weather when these things happens.
And then it has to be almost systemic. So almost dominant almost all over the body, at least extensive flush with all these sterile pustules that can come together and almost form lakes. Okay? Now, neutrophils are particularly important in this disease. So, you might find something called the spongy form posture, which are rich of neutrophils. And interestingly enough, these patients will have repeated occurrences. So if it's a first time, of course, that's not going to be there. But this is a chronic relapse in condition. And of course, a skin biopsy can always help. If you are in doubt, you can always biopsy that. But talk to your patients. See if they had this condition in the past about big range, up to 80%, but 30 to 80% of patients will have a relapse, and many of them experience one to three flares per year.
So, there's quite a few of them. And lastly, when you think of a patient with GPP, you think of a patient who has a lot of comorbidities. About 70% of these GPP patients have important comorbidities, and that's important not just in the diagnosis, but also in how we approach them. Why? Because these patients are just a little bit more delicate. They will have a higher risk of morbidity and mortality associated with GPP and their comorbidities, and therefore, some of the medication that we used to use for GPP, we have a lot of toxicities, might not be the best choice nowadays.
The IL-36 signaling axis has emerged as a critical driver of GPP pathogenesis. How has this discovery changed our understanding of the disease, and what implications does it have for future targeted therapies?
In my opinion, this has completely revolutionized how I think of the disease and probably how we as a specialty think of the disease. I mentioned to you before that some of the patients with GPP may have an underlying plaque psoriasis, but we now know that there are some overlaps in mechanism, but there are also some significant differences, and that's why the IL-36 becomes really important here. So we always knew that there was a lot of neutrophils. Think of the corneal wound healing and post-injury neovascularisation in neutrophils, but we now know that IL-36, it's important in diseases. And IL-36 is something that really attracts neutrophils. It's secret decreased, but is a lot of neutrophilic activities. It's part of the IL-1 super family. But that also brings in the factor of this systemic profound rapid inflammation with toll-like receptor activation. And that's why these patients tend to be acutely sick with fast progressing disease.
Now, not only we know that the importance of IL-36 signaling, but we also know that in some patients there are genetic mutations in the IL-36 receptors that makes them more prone to GPP and other pustular rashes, even caspase recruitment family member 14 (CARD14) or even tumor necrosis factor. But knowing about the IL-36 has really elucidated or unmasked a potential target in this disease that it's unique in GPP as compared to psoriasis where IL-17, IL-36, IL-23, I'm sorry, and TNF play a crucial role here. They do play an important role, and that's why we can have some clinical success by blockade of 23 or 17 and TNF. But we know that 36 is so important, even in patients who don't have the IL-36 receptor mutation, so independent of their mutation.
GPP flares can be triggered by a variety of factors, including infections, medication withdrawal, and hormonal changes. What strategies do you recommend for dermatologists to proactively manage and prevent these flares?
So, very important because we're in a time where, especially for GPP patients want to make sure that we talk to our patients, we create a patient education, the patient educations can range. We can talk to them about managing their stress and ways to manage their stress. And patients can learn how to cope with stress, whether they will be cognitive behavioral therapy, whatever you want to, but something to manage that stress. Additionally, for these GPP patients, more than many other dermatologic conditions, adherence to medication is important, but also careful withdrawal or stopping of medication. So it's not just taking your medication, but it's also you stop your medications with the number one example being corticosteroids. We know that withdrawal of corticosteroids patients may feel better at first when you start it, but the moment that you stop, they might have a dramatic and vigorous flare of their GPP, but there are also times of their life when they might be more susceptible to GPP flares.
Think about pregnancy, right? A special category. We always want to be careful, but we want to advise our patients who are planning on becoming pregnant have GPP, how this can be an important time for their GPP in terms of flares. And of course, mention to your patients and perhaps to the primary care and other specialists, emphasizing that this is perhaps a condition that requires more of a team approach rather than a single approach. How some medication can trigger that. Beta blockers, lithium, things that we think of psoriasis in many cases as potential medication triggers can also make GPP worse. But most importantly, and this is valuable for any inflammatory conditions, let's talk to our patients about diet and exercise. A healthy lifestyle will no matter what health this patient and for sure not hurt them because even though there might be a trigger in many cases, it's difficult to find the trigger. We have common ones that we talk about, and what I like to say to my patients is that, I know GPP may be better than you do, but you know your GPP better than I do. So if you know of a trigger, think about it. But if you have any sign of infections, let somebody know. Early treatment, early even prevention, even think of vaccines. Remember, vaccine can trigger GPP, but can prevent an infection, right? Can be important in these patients.
With ongoing advancements in immunomodulatory treatments, what are the most promising emerging therapies for GPP, and how should dermatologists prepare for their integration into clinical practice?
This was a field that we were treating very similar to psoriasis for us for many, many decades, whether it was with small molecule methotrexate, cyclosporine, retinoids, which had a lot of potential toxicities for these patients with a lot of comorbidities. And then in the era of biologics, multiple reports of success with 23 TNF or 17 inhibition. 2022 changed the field year because we had the first medication that was specifically approved for this, specifically target for this. And of course that was PGOs. Now that's why it's important to be on, to keep up with the new medications because it did bring a really new medication to the field. Now that approval really changed clinical practice. Now we have something FDA approved, not only for flare management, but also for the chronic recurrence to prevent those flares. Now, those clinical trials, of course, really establish the safety and efficacy of spesolimab, but there are other therapies., of course, that are upcoming.
Now we have data approval, so we want to base it on that. But there are other things on the horizon for our patients. Now IL-36, it's what we know it's important. We know that another monoclonal antibody called Imsidolimab has been studied in phase trial, clinical trial phase 2 at the GALLUP study, and with positive top line phase 3 in the GEMINI study. So we might have another one in the near future. But looking beyond the IL-36 receptor, we do have IL-36 gamma small molecules, a little bit different being developed. That's called ambrisentan, and that's in development, of course, but we do have other medications that, for example, have been studied for psoriasis, and I'm talking about something called a Type-2 inhibitor. Something called SOTYKTU that was investigated in phase 3 was an open label study. That's a poetic P SSO four study where there were three patients, I'm sorry, there 3 patients with GPP, and 2 out 3 did very well in there. So that has actually led to the inclusion of the treatment in the 2023 Japanese dermatology assessment guidelines for the treatment of GPP. We also have IL-1 inhibitors coming up, and those we mentioned earlier, IL-36 is part of the IL-1 super family. So we are going to keep our eyes open to see how those medications develop in this field.
Is there anything else you’d like to share with your colleagues regarding GPP?
Of course, as I tried to mention before, it is a complex disease for patients who tend to have a complex medical history. Now, it's one of those rare cases in dermatology where many of our patients might show up to an emergency room before they show up to us. They might have other specialists involved. So that's one disease where a team approach is more important. That's a disease where we really want to manage not just the GPP, but all the other comorbidities. Now having a monoclonal antibody that is being shown to be efficacious and safe is great, but we still want to involve other doctors who are part of the care, not only to know how the patient is doing, but also because some triggers can be avoided that way.