History of This Condition
Mal de Meleda (MdM), also known as Meleda disease and keratoderma palmoplantaris transgrediens of Siemens, is a rare autosomal recessive form of palmoplantar keratoderma (PPK), characterized by abnormal thickening of the skin of the palms and soles with extension to the dorsa of the hands and feet.1,2 The disease was first described by Stulli3 in 1826 on the island of Mljet (Meleda) in the Adriatic Sea, near the Dalmation coast in southernmost Croatia. Between the years 1397 and 1808, the island was evidently used to quarantine individuals suffering from plague and leprosy, which facilitated reproductive isolation and inbreeding.4 While the incidence of MdM in Meleda is approximately 1 in 200,5 additional cases have been reported from various other countries, prompting the suggestion that the disease allele may have originated outside of the island.6
A Note on Classification of Palmoplantar Keratodermas
Palmoplantar keratodermas (PPK) encompass a heterogeneous group of inherited and acquired disorders of keratinization that demonstrate thickening of the stratum corneum of the palms and soles, with or without additional dermatologic and extracutaneous manifestations. PPK may be subdivided based on clinical pattern, age at onset, mode of inheritance, transgrediens/progrediens behavior, histopathologic characteristics, and associated features.1,2,7 Transgrediens behavior indicates spread of the keratoderma to involve the dorsa of the hands and feet, while progrediens behavior signifies disease progression with age. Discrete grouping of the various types of PPK is not always possible, as several patients do not fall precisely into one of the different categories,7 and due to the extensive nomenclature of different PPK subtypes, grouping may vary between sources. Clinically, three patterns of PPK may be recognized1,2:
1. Diffuse PPK. This pattern is characterized by a symmetric hyperkeratosis involving the entire palm and sole, usually present at birth or within the first few months of life.
2. Focal PPK. This pattern is characterized by compact masses of keratin primarily on the feet and areas of repetitive mechanical trauma, but also involving the palms as well as skin at other sites.
3. Punctate PPK. This version is characterized by multiple drop-like keratoses which may be distributed over the entire palmoplantar surface or remain confined to smaller areas.
Simple PPK, in which disease involvement is limited to the skin, may be differentiated further from the complex keratodermas, which are forms of PPK associated with additional oral, nail, hair, sweat gland and dental anomalies.1 These abnormalities may accompany skin involvement as a result of their related embryonic origins from ectoderm and neuroectoderm.1 The syndromic keratodermas involve PPK associated with abnormalities of other organ systems, including deafness and cancer.1
Clinicopathologic Features of Mal de Meleda
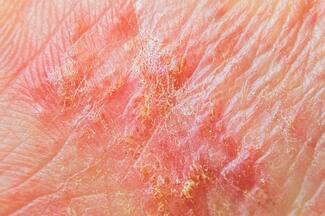
Mal de Meleda presents at birth or early infancy as a diffuse, symmetric, sharply demarcated palmoplantar keratoderma. Characteristically, lesions begin with erythematous scaling, and they progress to thickened yellow keratoses, with extended involvement of the dorsa of the hands and feet (transgrediens behavior) in a “glove-and-stocking” distribution.1,7 The disease may also demonstrate progrediens behavior, becoming more extensive with age,2,8 and mechanical trauma to affected skin may influence severity.4 Associated features can include knuckle pads, elbow and knee hyperkeratosis, brachydactyly, koilonychia, subungual hyperkeratosis, angular cheilitis, hyperhidrosis, pseudo-ainhum (autoamputation of the digits from constricting bands) and poor physical development.1,2 In a recent study of 39 patients with MdM, Ergin et al9 found nail abnormalities to be the most common associated feature (80%) followed by transgrediens PPK distribution, hand and foot edema, and conical tapering of the fingertips (60% each). Hyperhidrosis and maceration cause the development of a characteristic foul odor, which may become socially problematic for patients.4,8 Reports of malignant melanoma and squamous cell carcinoma arising in affected skin have also been published.10,11,12 Histologically, the epidermis of the palms and soles demonstrates orthokeratosis, acanthosis, and hypergranulosis, but no epidermolysis.1,6 Foci of parakeratosis along with a mild perivascular mononuclear cell infiltrate, as well as thickening of the papillary dermis, are also observed.7
Actinic elastosis and thickening of papillary blood vessel walls have been described as well.8 A report of MdM in a Taiwanese family8 showed a markedly lower percentage of T3 lymphocytes in the peripheral blood of both affected and unaffected family members when compared to controls. A moderately lower percentage of peripheral T4 cells and a decreased T4/T8 ratio were also noted. These findings may implicate a depressed cell-mediated immune response in the pathogenesis of the disease. Kuster et al13 demonstrated abnormal lipid patterns in the stratum corneum of several patients with different hereditary forms of PPK, including decreased amounts of total ceramides and increased amounts of free fatty acids. Increased levels of di- and triglycerides were also detected in the scales of two patients with MdM.
Genetics
Molecular linkage analysis has demonstrated strong evidence of a mutation located in the distal long arm of chromosome 8 (8qter).2,5 Affected individuals studied from the island of Meleda demonstrated homozygosity for a gene haplotype located telomeric to a region of chromosome 8 defined by the marker D8S1729.5 Studies of Algerian families14,15 also localized the defect to this chromosomal region, between or telomeric to markers D8S1751 and D8S1836. Three genes labeled E48, GML, and ARS (component B), which belong to a cluster of Ly-6/urokinase plasminogen activator (uPAR) genes involved in signal transduction, immune cell activation and cellular adhesion, reside within the identified interval on 8qter.16 A total of seven mutations, including homozygous deletion, nonsense and missense, in the ARS (component B) gene have been identified in families with MdM,17 resulting in abnormal production of SLURP-1, a cysteine-rich protein component of GPI-anchored glycoprotein receptors.16 Two recently identified defects involve a founder mutation (C99Y) in a Tunisian pedigree and a signal sequence mutation (W15R) in German and Scottish patients.17 It has been found that SLURP-1 potentiates the human alpha 7 nicotinic acetylcholine receptors present in keratinocytes, likely making it an essential neuromodulator for both epidermal homeostasis and inhibition of TNF-alpha release by macrophages during wound healing.18
Marrakchi et al identified several patients from Algeria, Tunisia, Croatia (including Meleda island), and Scotland who were found to be homozygous at two polymorphic sites for the mutation 82delT in the SLURP-1 gene and suggested the possibility of a founder effect spread by Serbo-Croatian sailors during the 14th to 17th centuries.17 Others19 disagree with this explanation, citing likely historical inaccuracies. An extensive description of the detailed genetics behind MdM is beyond the scope of this paper.
Differential Diagnosis
Mal de Meleda may be differentiated from other forms of PPK partly due to its transgrediens behavior. The basic table on page 63 further characterizes and separates multiple transgrediens variants of PPK using several distinct attributes. Eponyms for the various conditions have been omitted. Other hyperkeratotic conditions that must be differentiated from MdM include ichthyosis, psoriasis, lichen planus and mycosis fungoides.4
Managing This Condition
Oral retinoids are the mainstay of treatment for MdM, and many patients require long-term therapy.2,7 Oral etretinate and acitretin at approximately 0.5 to 1.0 mg/kg/day for adults and 0.5 mg/kg/day for children are both effective agents,2 but must be used judiciously in reproductive-age women due to possible long-term teratogenic effects. Dose-related side effects include cheilitis, mucosal dryness, epistaxis, urticarial or morbilliform eruptions, and alopecia.20 Reports have found Tigason (etretinate) more helpful in treating keratinization but less effective with associated erythema.8 However, this drug was removed from the U.S. market in 1998. The mechanism of action of oral retinoids in treating PPK has not been fully elucidated, but it has been suggested that they exert their effects in a late stage of epidermal differentiation,20 decreasing keratin production and causing disadherence between cells of the horny layer.21 Pseudo-ainhum development in MdM may be managed with retinoids or surgical correction (Z-plasty).1 Other treatments that have been employed, but were relatively ineffective, include topical salicylic acid, lactic acid and retinoic acid; topical corticosteroids; radiotherapy; and surgical excision.21
Carlos Rodriguez is a fourth-year medical student at the University of Illinois at Chicago College of Medicine, and Dr. Khachemoune, the Section Editor for “Derm Dx” is at the Wellman Center for Photomedicine, Department of Dermatology at Massachusetts General Hospital, Harvard Medical School in Boston, MA.
History of This Condition
Mal de Meleda (MdM), also known as Meleda disease and keratoderma palmoplantaris transgrediens of Siemens, is a rare autosomal recessive form of palmoplantar keratoderma (PPK), characterized by abnormal thickening of the skin of the palms and soles with extension to the dorsa of the hands and feet.1,2 The disease was first described by Stulli3 in 1826 on the island of Mljet (Meleda) in the Adriatic Sea, near the Dalmation coast in southernmost Croatia. Between the years 1397 and 1808, the island was evidently used to quarantine individuals suffering from plague and leprosy, which facilitated reproductive isolation and inbreeding.4 While the incidence of MdM in Meleda is approximately 1 in 200,5 additional cases have been reported from various other countries, prompting the suggestion that the disease allele may have originated outside of the island.6
A Note on Classification of Palmoplantar Keratodermas
Palmoplantar keratodermas (PPK) encompass a heterogeneous group of inherited and acquired disorders of keratinization that demonstrate thickening of the stratum corneum of the palms and soles, with or without additional dermatologic and extracutaneous manifestations. PPK may be subdivided based on clinical pattern, age at onset, mode of inheritance, transgrediens/progrediens behavior, histopathologic characteristics, and associated features.1,2,7 Transgrediens behavior indicates spread of the keratoderma to involve the dorsa of the hands and feet, while progrediens behavior signifies disease progression with age. Discrete grouping of the various types of PPK is not always possible, as several patients do not fall precisely into one of the different categories,7 and due to the extensive nomenclature of different PPK subtypes, grouping may vary between sources. Clinically, three patterns of PPK may be recognized1,2:
1. Diffuse PPK. This pattern is characterized by a symmetric hyperkeratosis involving the entire palm and sole, usually present at birth or within the first few months of life.
2. Focal PPK. This pattern is characterized by compact masses of keratin primarily on the feet and areas of repetitive mechanical trauma, but also involving the palms as well as skin at other sites.
3. Punctate PPK. This version is characterized by multiple drop-like keratoses which may be distributed over the entire palmoplantar surface or remain confined to smaller areas.
Simple PPK, in which disease involvement is limited to the skin, may be differentiated further from the complex keratodermas, which are forms of PPK associated with additional oral, nail, hair, sweat gland and dental anomalies.1 These abnormalities may accompany skin involvement as a result of their related embryonic origins from ectoderm and neuroectoderm.1 The syndromic keratodermas involve PPK associated with abnormalities of other organ systems, including deafness and cancer.1
Clinicopathologic Features of Mal de Meleda
Mal de Meleda presents at birth or early infancy as a diffuse, symmetric, sharply demarcated palmoplantar keratoderma. Characteristically, lesions begin with erythematous scaling, and they progress to thickened yellow keratoses, with extended involvement of the dorsa of the hands and feet (transgrediens behavior) in a “glove-and-stocking” distribution.1,7 The disease may also demonstrate progrediens behavior, becoming more extensive with age,2,8 and mechanical trauma to affected skin may influence severity.4 Associated features can include knuckle pads, elbow and knee hyperkeratosis, brachydactyly, koilonychia, subungual hyperkeratosis, angular cheilitis, hyperhidrosis, pseudo-ainhum (autoamputation of the digits from constricting bands) and poor physical development.1,2 In a recent study of 39 patients with MdM, Ergin et al9 found nail abnormalities to be the most common associated feature (80%) followed by transgrediens PPK distribution, hand and foot edema, and conical tapering of the fingertips (60% each). Hyperhidrosis and maceration cause the development of a characteristic foul odor, which may become socially problematic for patients.4,8 Reports of malignant melanoma and squamous cell carcinoma arising in affected skin have also been published.10,11,12 Histologically, the epidermis of the palms and soles demonstrates orthokeratosis, acanthosis, and hypergranulosis, but no epidermolysis.1,6 Foci of parakeratosis along with a mild perivascular mononuclear cell infiltrate, as well as thickening of the papillary dermis, are also observed.7
Actinic elastosis and thickening of papillary blood vessel walls have been described as well.8 A report of MdM in a Taiwanese family8 showed a markedly lower percentage of T3 lymphocytes in the peripheral blood of both affected and unaffected family members when compared to controls. A moderately lower percentage of peripheral T4 cells and a decreased T4/T8 ratio were also noted. These findings may implicate a depressed cell-mediated immune response in the pathogenesis of the disease. Kuster et al13 demonstrated abnormal lipid patterns in the stratum corneum of several patients with different hereditary forms of PPK, including decreased amounts of total ceramides and increased amounts of free fatty acids. Increased levels of di- and triglycerides were also detected in the scales of two patients with MdM.
Genetics
Molecular linkage analysis has demonstrated strong evidence of a mutation located in the distal long arm of chromosome 8 (8qter).2,5 Affected individuals studied from the island of Meleda demonstrated homozygosity for a gene haplotype located telomeric to a region of chromosome 8 defined by the marker D8S1729.5 Studies of Algerian families14,15 also localized the defect to this chromosomal region, between or telomeric to markers D8S1751 and D8S1836. Three genes labeled E48, GML, and ARS (component B), which belong to a cluster of Ly-6/urokinase plasminogen activator (uPAR) genes involved in signal transduction, immune cell activation and cellular adhesion, reside within the identified interval on 8qter.16 A total of seven mutations, including homozygous deletion, nonsense and missense, in the ARS (component B) gene have been identified in families with MdM,17 resulting in abnormal production of SLURP-1, a cysteine-rich protein component of GPI-anchored glycoprotein receptors.16 Two recently identified defects involve a founder mutation (C99Y) in a Tunisian pedigree and a signal sequence mutation (W15R) in German and Scottish patients.17 It has been found that SLURP-1 potentiates the human alpha 7 nicotinic acetylcholine receptors present in keratinocytes, likely making it an essential neuromodulator for both epidermal homeostasis and inhibition of TNF-alpha release by macrophages during wound healing.18
Marrakchi et al identified several patients from Algeria, Tunisia, Croatia (including Meleda island), and Scotland who were found to be homozygous at two polymorphic sites for the mutation 82delT in the SLURP-1 gene and suggested the possibility of a founder effect spread by Serbo-Croatian sailors during the 14th to 17th centuries.17 Others19 disagree with this explanation, citing likely historical inaccuracies. An extensive description of the detailed genetics behind MdM is beyond the scope of this paper.
Differential Diagnosis
Mal de Meleda may be differentiated from other forms of PPK partly due to its transgrediens behavior. The basic table on page 63 further characterizes and separates multiple transgrediens variants of PPK using several distinct attributes. Eponyms for the various conditions have been omitted. Other hyperkeratotic conditions that must be differentiated from MdM include ichthyosis, psoriasis, lichen planus and mycosis fungoides.4
Managing This Condition
Oral retinoids are the mainstay of treatment for MdM, and many patients require long-term therapy.2,7 Oral etretinate and acitretin at approximately 0.5 to 1.0 mg/kg/day for adults and 0.5 mg/kg/day for children are both effective agents,2 but must be used judiciously in reproductive-age women due to possible long-term teratogenic effects. Dose-related side effects include cheilitis, mucosal dryness, epistaxis, urticarial or morbilliform eruptions, and alopecia.20 Reports have found Tigason (etretinate) more helpful in treating keratinization but less effective with associated erythema.8 However, this drug was removed from the U.S. market in 1998. The mechanism of action of oral retinoids in treating PPK has not been fully elucidated, but it has been suggested that they exert their effects in a late stage of epidermal differentiation,20 decreasing keratin production and causing disadherence between cells of the horny layer.21 Pseudo-ainhum development in MdM may be managed with retinoids or surgical correction (Z-plasty).1 Other treatments that have been employed, but were relatively ineffective, include topical salicylic acid, lactic acid and retinoic acid; topical corticosteroids; radiotherapy; and surgical excision.21
Carlos Rodriguez is a fourth-year medical student at the University of Illinois at Chicago College of Medicine, and Dr. Khachemoune, the Section Editor for “Derm Dx” is at the Wellman Center for Photomedicine, Department of Dermatology at Massachusetts General Hospital, Harvard Medical School in Boston, MA.
History of This Condition
Mal de Meleda (MdM), also known as Meleda disease and keratoderma palmoplantaris transgrediens of Siemens, is a rare autosomal recessive form of palmoplantar keratoderma (PPK), characterized by abnormal thickening of the skin of the palms and soles with extension to the dorsa of the hands and feet.1,2 The disease was first described by Stulli3 in 1826 on the island of Mljet (Meleda) in the Adriatic Sea, near the Dalmation coast in southernmost Croatia. Between the years 1397 and 1808, the island was evidently used to quarantine individuals suffering from plague and leprosy, which facilitated reproductive isolation and inbreeding.4 While the incidence of MdM in Meleda is approximately 1 in 200,5 additional cases have been reported from various other countries, prompting the suggestion that the disease allele may have originated outside of the island.6
A Note on Classification of Palmoplantar Keratodermas
Palmoplantar keratodermas (PPK) encompass a heterogeneous group of inherited and acquired disorders of keratinization that demonstrate thickening of the stratum corneum of the palms and soles, with or without additional dermatologic and extracutaneous manifestations. PPK may be subdivided based on clinical pattern, age at onset, mode of inheritance, transgrediens/progrediens behavior, histopathologic characteristics, and associated features.1,2,7 Transgrediens behavior indicates spread of the keratoderma to involve the dorsa of the hands and feet, while progrediens behavior signifies disease progression with age. Discrete grouping of the various types of PPK is not always possible, as several patients do not fall precisely into one of the different categories,7 and due to the extensive nomenclature of different PPK subtypes, grouping may vary between sources. Clinically, three patterns of PPK may be recognized1,2:
1. Diffuse PPK. This pattern is characterized by a symmetric hyperkeratosis involving the entire palm and sole, usually present at birth or within the first few months of life.
2. Focal PPK. This pattern is characterized by compact masses of keratin primarily on the feet and areas of repetitive mechanical trauma, but also involving the palms as well as skin at other sites.
3. Punctate PPK. This version is characterized by multiple drop-like keratoses which may be distributed over the entire palmoplantar surface or remain confined to smaller areas.
Simple PPK, in which disease involvement is limited to the skin, may be differentiated further from the complex keratodermas, which are forms of PPK associated with additional oral, nail, hair, sweat gland and dental anomalies.1 These abnormalities may accompany skin involvement as a result of their related embryonic origins from ectoderm and neuroectoderm.1 The syndromic keratodermas involve PPK associated with abnormalities of other organ systems, including deafness and cancer.1
Clinicopathologic Features of Mal de Meleda
Mal de Meleda presents at birth or early infancy as a diffuse, symmetric, sharply demarcated palmoplantar keratoderma. Characteristically, lesions begin with erythematous scaling, and they progress to thickened yellow keratoses, with extended involvement of the dorsa of the hands and feet (transgrediens behavior) in a “glove-and-stocking” distribution.1,7 The disease may also demonstrate progrediens behavior, becoming more extensive with age,2,8 and mechanical trauma to affected skin may influence severity.4 Associated features can include knuckle pads, elbow and knee hyperkeratosis, brachydactyly, koilonychia, subungual hyperkeratosis, angular cheilitis, hyperhidrosis, pseudo-ainhum (autoamputation of the digits from constricting bands) and poor physical development.1,2 In a recent study of 39 patients with MdM, Ergin et al9 found nail abnormalities to be the most common associated feature (80%) followed by transgrediens PPK distribution, hand and foot edema, and conical tapering of the fingertips (60% each). Hyperhidrosis and maceration cause the development of a characteristic foul odor, which may become socially problematic for patients.4,8 Reports of malignant melanoma and squamous cell carcinoma arising in affected skin have also been published.10,11,12 Histologically, the epidermis of the palms and soles demonstrates orthokeratosis, acanthosis, and hypergranulosis, but no epidermolysis.1,6 Foci of parakeratosis along with a mild perivascular mononuclear cell infiltrate, as well as thickening of the papillary dermis, are also observed.7
Actinic elastosis and thickening of papillary blood vessel walls have been described as well.8 A report of MdM in a Taiwanese family8 showed a markedly lower percentage of T3 lymphocytes in the peripheral blood of both affected and unaffected family members when compared to controls. A moderately lower percentage of peripheral T4 cells and a decreased T4/T8 ratio were also noted. These findings may implicate a depressed cell-mediated immune response in the pathogenesis of the disease. Kuster et al13 demonstrated abnormal lipid patterns in the stratum corneum of several patients with different hereditary forms of PPK, including decreased amounts of total ceramides and increased amounts of free fatty acids. Increased levels of di- and triglycerides were also detected in the scales of two patients with MdM.
Genetics
Molecular linkage analysis has demonstrated strong evidence of a mutation located in the distal long arm of chromosome 8 (8qter).2,5 Affected individuals studied from the island of Meleda demonstrated homozygosity for a gene haplotype located telomeric to a region of chromosome 8 defined by the marker D8S1729.5 Studies of Algerian families14,15 also localized the defect to this chromosomal region, between or telomeric to markers D8S1751 and D8S1836. Three genes labeled E48, GML, and ARS (component B), which belong to a cluster of Ly-6/urokinase plasminogen activator (uPAR) genes involved in signal transduction, immune cell activation and cellular adhesion, reside within the identified interval on 8qter.16 A total of seven mutations, including homozygous deletion, nonsense and missense, in the ARS (component B) gene have been identified in families with MdM,17 resulting in abnormal production of SLURP-1, a cysteine-rich protein component of GPI-anchored glycoprotein receptors.16 Two recently identified defects involve a founder mutation (C99Y) in a Tunisian pedigree and a signal sequence mutation (W15R) in German and Scottish patients.17 It has been found that SLURP-1 potentiates the human alpha 7 nicotinic acetylcholine receptors present in keratinocytes, likely making it an essential neuromodulator for both epidermal homeostasis and inhibition of TNF-alpha release by macrophages during wound healing.18
Marrakchi et al identified several patients from Algeria, Tunisia, Croatia (including Meleda island), and Scotland who were found to be homozygous at two polymorphic sites for the mutation 82delT in the SLURP-1 gene and suggested the possibility of a founder effect spread by Serbo-Croatian sailors during the 14th to 17th centuries.17 Others19 disagree with this explanation, citing likely historical inaccuracies. An extensive description of the detailed genetics behind MdM is beyond the scope of this paper.
Differential Diagnosis
Mal de Meleda may be differentiated from other forms of PPK partly due to its transgrediens behavior. The basic table on page 63 further characterizes and separates multiple transgrediens variants of PPK using several distinct attributes. Eponyms for the various conditions have been omitted. Other hyperkeratotic conditions that must be differentiated from MdM include ichthyosis, psoriasis, lichen planus and mycosis fungoides.4
Managing This Condition
Oral retinoids are the mainstay of treatment for MdM, and many patients require long-term therapy.2,7 Oral etretinate and acitretin at approximately 0.5 to 1.0 mg/kg/day for adults and 0.5 mg/kg/day for children are both effective agents,2 but must be used judiciously in reproductive-age women due to possible long-term teratogenic effects. Dose-related side effects include cheilitis, mucosal dryness, epistaxis, urticarial or morbilliform eruptions, and alopecia.20 Reports have found Tigason (etretinate) more helpful in treating keratinization but less effective with associated erythema.8 However, this drug was removed from the U.S. market in 1998. The mechanism of action of oral retinoids in treating PPK has not been fully elucidated, but it has been suggested that they exert their effects in a late stage of epidermal differentiation,20 decreasing keratin production and causing disadherence between cells of the horny layer.21 Pseudo-ainhum development in MdM may be managed with retinoids or surgical correction (Z-plasty).1 Other treatments that have been employed, but were relatively ineffective, include topical salicylic acid, lactic acid and retinoic acid; topical corticosteroids; radiotherapy; and surgical excision.21
Carlos Rodriguez is a fourth-year medical student at the University of Illinois at Chicago College of Medicine, and Dr. Khachemoune, the Section Editor for “Derm Dx” is at the Wellman Center for Photomedicine, Department of Dermatology at Massachusetts General Hospital, Harvard Medical School in Boston, MA.