Treating Chronic Lower Extremity Ulcers With Autologous Skin Grafting
Wound care providers have long been challenged by chronic leg and foot ulcers due to difficulty in healing these wounds. The pain and other physical and psychological effects of these wounds often lead to a significantly reduced quality of life for patients.1 Chronic wound treatments also cause a great financial burden to patients and the health care system. In the United States alone there are more than 6 million cases of chronic wounds a year at a staggering cost of $25 billion.2 While there are many options for treating chronic foot and leg ulcers, there is also a need for new treatment methods that can promote a higher rate of successful healing with fewer side effects.
A well-established wound treatment involves grafting harvested autologous skin and applying it to a properly debrided ulcer to stimulate healing. Autologous skin grafting is considered the gold standard for treating chronic wounds3 due to the use of the patient’s own skin to help promote healing. There are several methods to harvest epidermal/dermal sheets with the most common being the use of a split-thickness skin graft.
Harvesting split-thickness skin grafts requires skill and precision. Additionally, the associated equipment may not produce a graft with the precise thickness of skin needed. This technique also creates a new dermal wound at the donor site that needs special care and attention, with risk for chronicity, pain, or long-term treatment.
An effective alternative harvesting method is using suction blisters to produce an epidermal skin graft.4-6 Using a specialized negative pressure vacuum chamber placed directly on the donor skin, the clinician cleaves the epidermis from the underlying dermis to create a blister. One can then easily harvest the raised epidermal blister roof by carefully dissecting around the graft periphery. With this method, the patient experiences minimal discomfort and the donor site heals very rapidly compared to split-thickness skin graft harvesting.7 One downside of suction blisters in the past is the long blister formation time, which can be 2 hours or longer.8 However, new technology that introduces a mild heat source within a negative pressure chamber has shown to significantly reduce blister formation time.
For this case series, we used the Epitech system (TARA Medical Devices LLC) to prepare the blisters from which we harvested the epidermal sheets. In our experience, this system safely creates blisters in a fast, controlled and predictable manner. Precisely regulated suction and a proprietary heating profile help prepare viable epidermal tissue with a typical formation time of only 30–45 minutes based on our observations. This particular harvesting system also incorporates features to reduce patient discomfort as blisters form. We find that anesthesia is usually not required and was not used with patients in this case series.
A Closer Look at the Patients in the Case Series
This case series focused on 10 patients at the Fisher-Titus Wound Healing Center in Norwalk, Ohio. Wounds in the 10 patients consisted of 5 diabetic ulcers, 3 venous stasis ulcers, 1 pressure ulcer and 1 traumatic ulcer (see Table 1). The clinicians harvested epidermal tissue for autologous grafting of the ulcers using the technique described below and the above-mentioned harvesting system. We defined a healed wound as 100% epithelialization with no drainage.

Comorbidities: CVI—Chronic Venous Insufficiency, CVA—Cerebrovascular Accident (stroke),
COPD—Chronic Obstructive Pulmonary Disease, T1D—Type 1 Diabetes, T2D—Type 2 Diabetes
Wound preparation. After measuring and photographing the wound, surgeons thoroughly debrided the ulcer to assist in the removal of local barriers to healing and to promote granulation tissue. Debridement consisted of using curettes and blades, and dead tissue removal was via forceps and scissors.
Donor site location and preparation. An area of unexposed skin, such as the inner thigh region, was the donor site. Unexposed skin is preferable, as testing performed by the manufacturer and confirmed by physicians using the system found that areas exposed to sunlight typically have longer blister formation times. Surgeons prepared the donor site by scrubbing with a chlorhexidine gluconate solution and further sanitized by wiping with an alcohol pad.
Epidermal harvesting. Surgeons used the above-mentioned system at the donor site to produce several blisters 1cm in diameter. The number of 1cm blisters produced de-pended on the size of the wound and was typically 4 to 6 blisters. After blister formation, surgeons removed the donor epidermis from the perimeter with careful dissection with a 15-blade and forceps. Surgeons then carefully transferred the epidermal grafts onto a small non-adherent dressing with the use of forceps, taking care to place the grafts with the dorsal moist surface of the graft face up on the dressing. Surgeons then applied the dressing to the ulcer with the dermal side of the grafts touching the wound surface and secured the dressing utilizing wound closure strips.
Post-procedure. After placing the epidermal sheets on the wound, surgeons covered the area with 2x2 inch or 4x4 inch sterile gauze dressing and a thicker-type gauze or cast padding, dressing followed by a compressive bandage. The patients received instructions to keep the dressings dry and covered until their follow-up visit in one week with appropriate offloading of the site if warranted.
The clinicians covered the donor site with a 2x2 inch sterile gauze and a transparent film dressing which remained in place for 1 to 2 days, after which surgeons removed the dressing. The patient received instructions to cleanse the wound and use a gauze bandage daily until the wound was healed, usually in 7–10 days.
Patient follow-up. The patients were to return to the clinic for evaluation, at which time surgeons measured and photographed the wounds for the purpose of this study.
Results
The patient demographics and wound information are summarized in Table 1.

Patient 1. A 62-year-old male presented with a diabetic ulcer in the right foot. He had a history of type 2 diabetes and coronary artery disease. The epidermal harvesting procedure occurred on 3/15/23. On 3/15/23 (left photo above) wound measurements were 1.4cm x 0.6cm x 0.2cm. On 4/19/23 (right photo above) wound measurements were 0cm x 0cm x 0cm.

Patient 2. A 59-year-old male presented with a diabetic foot ulcer in the right great toe. He had a history of type 2 diabetes and osteomyelitis. The epidermal harvesting procedure occurred on 3/21/23. On 3/21/23 (left photo above) wound measurements were 1.0cm x 0.2cm, x 0.4cm. On 4/04/23 wound measurements were 0cm x 0cm x 0cm.

Patient 3. A 35-year-old female presented with a diabetic foot ulcer in the left second toe. She had a history of type 1 diabetes and obesity. The epidermal harvesting procedure occurred on 3/22/23. On 3/22/23 (left photo above) wound measurements were 0.6cmx 0.6cm x 0.3cm. On 5/03/23 (right photo above) wound measurements were 0cm x 0cm x 0cm.

Patient 4. A 67-year-old female presented with a pressure ulcer in the left heel. She had a history of cardiovascular accident, chronic obstructive pulmonary disease (COPD), and Parkinson’s disease. The epidermal harvesting procedure occurred on 3/22/23. On 3/22/23 (left photo above) wound measurements were 0.6cm x 0.6cm x 0.3cm. On 4/5/23 (right photo above), wound measurements were 0cm x 0cm x 0cm.

Patient 5. A 59-year-old male presented with a right diabetic foot ulcer. He had a history of type 2 diabetes and rheumatoid arthritis. The epidermal harvesting procedure occurred on 3/22/23. On 3/22/23 (left photo above) wound measurements were 1.0cm x 0.2cm x 0.3cm. On 4/5/23 (right photo above) wound measurements were 0cm x 0cm x 0cm.

Patient 6. An 81-year-old female presented with a venous stasis ulcer in the right ankle. She had a history of chronic venous insufficiency, COPD and morbid obesity. The epidermal harvesting procedure occurred on 2/22/23. On 2/22/23 (left photo above) wound measurement was length 2.0cm, width 0.4cm, depth 0.1cm. On 3/15/23 (right photo above), wound measurements were 0.4cm x 0.4cm x 0.1cm. On 5/3/23 wound measurements were 0cm x 0cm x 0cm.

Patient 7. A 69-year-old male presented with a venous stasis ulcer in the right ankle. He had a history of chronic venous insufficiency and leg paresthesia. The epidermal harvesting procedure occurred on 3/01/23. On 3/1/23 (left photo above) wound measurements were 0.6cm x 0.6cm x 0.1cm. On 3/29/23 (right photo above) wound measurements were 0cm x 0cm x 0cm.

Patient 8. A 92-year-old female presented with an ulcer in the right lower leg due to trauma. She had a history of coronary artery disease. The epidermal harvesting procedure occurred on 3/07/23. On 3/7/23 (left photo above) wound measurements were 1.8cm x 0.8cm x 0.1cm. On 4/25/23 (right photo above) wound measurements were 0cm x 0cm x 0cm.
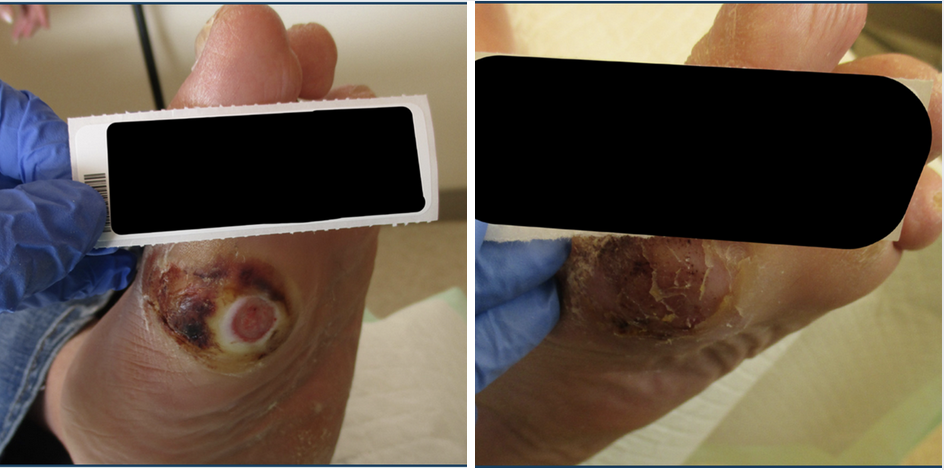
Patient 9. A 79-year-old female presented with a diabetic foot ulcer in the left great toe. She had a history of type 2 diabetes, chronic kidney disease and congestive heart failure. The epidermal harvesting procedure occurred on 3/07/23. On 3/7/23 (left photo above) wound measurements were 1.2cm x 1.2cm x 0.2cm. On 6/6/23 (right photo above) wound measurements were 0cm x 0cm x 0cm.

Patient 10. A 57-year-old female presented with a venous stasis ulcer in the left lower extremity. She had a history of chronic venous insufficiency, type 2 diabetes and COPD. The epidermal harvesting procedure occurred on 3/08/23. On 3/8/23 wound measurements were 1.0cm x 0.5cm x 0.2cm. On 3/33/23 wound measurements were 0cm x 0cm x 0cm.
What You Should Know About the Skin Grafting Procedure
Skin grafting is a well-established method to promote healing of chronic, non-healing wounds. Split-thickness grafts are most commonly used for this procedure and consist of both epidermis and dermis. Harvesting of split-thickness grafts requires excising skin at the level of the dermis, leaving a wound that heals by secondary intention. The wound left by harvesting itself can be problematic, potentially causing pain and delayed wound healing. Furthermore, the donor site is left with a permanent scar, which can be disfiguring. While surgeons have used pure epidermal grafts successfully to treat chronic wounds, the creation and harvesting of pure epidermal grafts is difficult and time consuming. In this small case series, a new skin harvesting system created suction blisters that were used as epidermal grafts to treat non-healing wounds. We found that the advantage of this technique is the relatively short time to produce the blisters and minimal discomfort involved. Additionally, minimal scarring remained at the donor site due to the fact the dermis is not disrupted during the procedure.
The procedure was successful in our series, with all 10 patients having excellent healing of their wounds with this technique. A limitation of this series is lack of a control group and variability in patient age, diagnosis, previous treatment, and wound size. Our purpose was to perform a small proof-of-concept study to determine if this technique could be successful. While a 100% healing rate may not be possible for all patients, our results from this small case series suggest that the skin harvesting system used has excellent potential for the treatment of chronic leg and foot ulcers and further studies are warranted.
Marc D. Dolce, DPM, FACFAS is board certified in foot surgery by the American Board of Foot and Ankle Surgery. Dr. Dolce’s professional interests are in the area of diabetic limb salvage surgery as well as reconstructive foot and ankle surgery. Dr. Dolce primarily practices at NOMS Northern Ohio Foot & Ankle Specialists in Norwalk, Ohio.
Nicholas A. Brown, DPM, FACFAS is board certified in foot surgery by the American Board of Podiatric Surgery. His professional interests include advanced diabetic wound care techniques and treatments as well as reconstructive foot and ankle surgery. Dr. Brown primarily practices at NOMS Northern Ohio Foot & Ankle in Sandusky, Ohio.
Kareem R. Dolce, DPM, FACFAS is board certified in foot surgery by the American Board of Foot and Ankle Surgery. Areas of specialty include forefoot and rearfoot reconstructive surgery, diabetic wound care and pediatric foot conditions. Dr. Dolce primarily practices at NOMS Northern Ohio Foot & Ankle Specialists in Norwalk, Ohio.
References
1. Hopman WM, Buchanan M, VanDenKerkhof EG, Harrison MB. Pain and health-related quality of life in people with chronic leg ulcers. Chronic Dis Inj Can. 2013;33(3):167-74.
2. Brem H, Stojadinovic O, Diegelmann RF, et al. Molecular markers in patients with chronic wounds to guide surgical debridement. Mol Med. 2007;13(1-2):30-9. doi: 10.2119/2006-00054.
3. Kianian S, Zhao K, Kaur J, et al. Autologous skin grafts, versus tissue-engineered skin constructs: a systematic review and meta-analysis. Plast Reconstr Surg Glob Open. 2023;11(6):e5100. doi: 10.1097/GOX.0000000000005100.
4. Costanzo U, Streit M, Braathen LR. Autologous suction blister grafting for chronic leg ulcers. J Eur Acad Dermatol Venereol. 2008;22(1):7-10. doi: 10.1111/j.1468-3083.2007.02148.x.
5. Saydam M, Yilmaz KB, Bostanci MT, et al. The use of autologous epidermal grafts for diabetic foot ulcer emergencies: A clinical study. Ulus Travma Acil Cerrahi Derg. 2022;28:262-267.
6. Hentzer B, Kobayasi T. Suction blister transplantation for leg ulcers. Acta Derm Venereol. 1975;55(3):207-9.
7. Kanapathy M, Hachach-Haram N, Bystrzonowski N, Harding K, Mosahebi A, Richards T. Epidermal grafting versus split-thickness skin grafting for wound healing (EPIGRAAFT): study protocol for a randomised controlled trial. Trials. 2016;17(1):245. doi: 10.1186/s13063-016-1352-y.
8. AlJasser MI. Faster suction blister formation using 2 hair dryers. J Am Acad Dermatol. 2018 Jun;78(6):e153-e154. doi: 10.1016/j.jaad.2017.12.037.











