Examining the Root Cause of Hallux Valgus
Patients with hallux abductovalgus deformity (HAV) may commonly ask their doctor, “What caused my bunion?” When posed this question, does your response restate a long-held notion that bunions have multiple causes? Or do you share a growing belief that there is a single “root cause” of a bunion located at the first tarsometatarsal (TMT) joint?
The notion of a “root cause” of HAV deformity emerged in a series of publications from a group of researchers beginning in 2013.1,2 These papers described a new “triplane correction” of HAV deformity involving arthrodesis of the first TMT joint. Dayton and colleagues cite the center of rotation of angulation (CORA) concept described by Paley3 and state, “In the case of a bunion, the primary etiology is the deformed anatomy or the level of deformity. We find the level of deformity at the metatarsal cuneiform joint.”2 This notion proposes that the first metatarsocuneiform joint (MCJ) has deformed anatomy and is the location of the CORA in HAV deformity.
Previous studies have identified 2 CORA locations in HAV deformity.4,5 The angulation between the first metatarsal and the proximal phalanx of the hallux creates the first apex of deformity, and the angulation between the first and second metatarsal creates the second apex of deformity. Neither of these 2 apices are located at the first TMT joint. One CORA is located in the distal portion of the first metatarsal and the other CORA is located near the naviculocuneiform joint. Apart from axis of angulation location, proponents of the triplane Lapidus procedure argue that the first TMT joint is the location where triplane rotation deformity originates.2
The recognition of a third plane of HAV deformity is based upon studies that document pronation rotation of the first metatarsal, which those authors assert is present in most patients with HAV deformity.6-9 Some researchers believe that frontal plane rotation of the first metatarsal combined with sagittal plane dorsiflexion and transverse plane adduction not only takes place at first TMT joint, but actually creates a single root cause of a bunion.10 This belief that all 3 planes of HAV deformity originate from a single joint deserves further scrutiny based on recent research findings.
Does Sagittal Plane Deformity of the First Ray Originate From the First TMT Joint?
The concept of sagittal plane instability specifically at the first TMT joint is often blurred with the condition known as “hypermobility” of the entire first ray of the foot.11 Studies implicate excessive dorsal mobility of the first TMT joint as a cause of HAV deformity.12-14 These early reports advocated arthrodesis of the first TMT joint to address sagittal plane hypermobility.
There is no universally agreed-upon definition of first ray hypermobility. Meyr, using a validated testing instrument, demonstrated that sagittal plane motion of the first ray is a continuous variable with no specific threshold for hypermobility.15 Shibuya and colleagues conducted a systematic review of all studies of first ray mobility comparing patients with HAV and healthy controls.16 Meta-analysis of the data from those studies revealed that patients with HAV deformity have a significant, 3.6 mm greater range of dorsal excursion of the first ray compared to healthy controls.16
It is important to note that the studies reviewed by Shibuya and colleagues measured dorsal excursion of the first metatarsal when the foot was held in a static position. Furthermore, the measured motion was contributed to by all 3 joints of the medial column, not just the first TMT joint. Finally, measures of first ray motion in a static foot do not reflect actual motion which occurs during dynamic gait. Allen and colleagues found no correlations between first ray motion measured in the static condition compared to actual motion of this segment during dynamic gait.17
Researchers have challenged hypermobility of the first ray as a cause of HAV. Several studies show that realignment osteotomy of the first metatarsal to correct HAV deformity will reduce the magnitude of presurgical dorsal excursion of the first ray by up to 50%.18-22 After conducting extensive research on this topic, Doty and Coughlin state, “Metatarsocuneiform joint mobility may be necessary for a hallux valgus deformity to develop; however, “hypermobility” may not be the cause but rather the result of a hallux valgus deformity.”23
Sagittal plane stability of the metatarsals is dependent upon anatomic structures located distally at the metatarsophalangeal (MTP) joint. Research has demonstrated the important role of the flexor hallucis longus, the plantar fascia, and the structures attaching to the sesamoid apparatus to stabilize the head of the first metatarsal on the ground during terminal stance.24-26 Adduction and frontal plane rotation of the head of the first metatarsal as HAV deformity progresses compromises the dynamic stiffening mechanism provided by the flexor hallucis longus tendon, the plantar fascia via the windlass mechanism, and intrinsic muscles inserting on the sesamoids at the first MTP joint.27 This loss of shielding from ground reaction forces at the head of the first metatarsal will lead to excessive dorsal mobility in the proximal joints of the first ray, including the first TMT.20,27
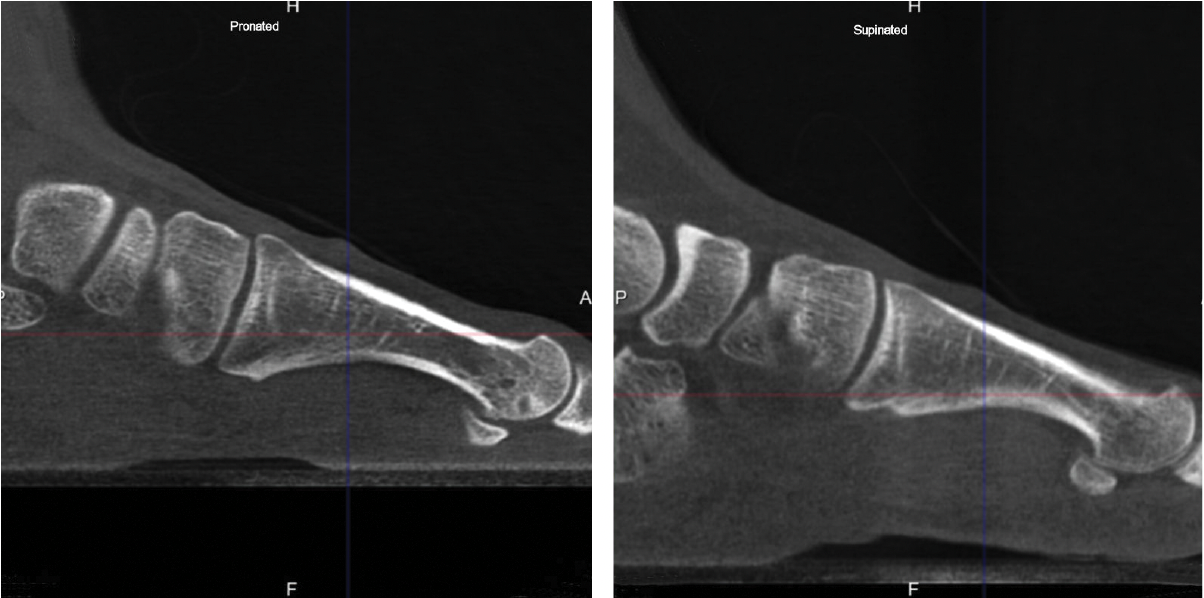
Indeed, authors have demonstrated evidence of acquired sagittal plane instability of the first TMT in HAV patients using various techniques. Weight-bearing radiographs reveal plantar gapping and dorsal translation of the first TMT joint.28 These findings have been replicated in simulated weight-bearing computed tomography (CT) imaging studies as well as true weight-bearing CT (WBCT) studies that show plantar gapping and dorsal translation of the first metatarsal at the first TMT joint in HAV patients (Figures 1A,B).29-30

A gait study using 3-dimensional motion capture showed that patients with HAV deformity had plantar displacement of the medial cuneiform and dorsal shift of the first metatarsal at the first TMT joint. This dynamic study showed that dorsal translation of the first TMT joint increased with severity of hallux valgus deformity, suggesting this was a reactive, rather than causative, mechanism.31
While researchers have demonstrated the presence of sagittal plane instability of the first TMT joint in HAV patients, there is no evidence to date that this condition is a predisposing factor or a “root cause” of formation of a bunion deformity. Sagittal plane stability of the first metatarsal relies on dynamic soft tissue restraints located at the first MTP joint.24-27 In regards to first ray sagittal stability in HAV deformity, Doty and Coughlin state “We believe that alignment confers stability, rather than instability leads to malalignment.”20

Is First Metatarsal Pronation the Root Cause of a Bunion?
Studies have implicated first metatarsal pronation as a primary etiology of HAV deformity.8,32-35 However, these reports did not identify which joint or joints in the medial column contribute to a pronated position of the first metatarsal. Furthermore, the specific role that first metatarsal pronation plays in the pathogenesis of HAV remains poorly understood.
It appears from published studies using true weight-bearing CT imaging that normal healthy individuals can have a pronated position of the first metatarsal which is of equal or greater magnitude than individuals with HAV deformity.36,37 Mahamoud and colleagues found no difference in magnitude of frontal plane pronation of the head of the first metatarsal in HAV patients compared to healthy controls.38 In 2 WBCT studies, Lalevée and colleagues observed a paradoxical supination motion of the first ray as HAV deformity increased, adding further controversy to the role of pronation rotation of the first metatarsal in the pathomechanics of HAV.39,40
Studies have shown that there is no correlation between the magnitude of HAV deformity, as measured with hallux abductus angle and intermetatarsal angle, and the magnitude of first metatarsal pronation rotation. Thus, pronation rotation of the first metatarsal could not be considered the root cause of HAV deformity. More appropriately, one should consider a pronated position of the head of the first metatarsal relative to the supportive surface to be a risk factor for the occurrence and recurrence of a bunion deformity.39,41

Is a Pronated Position of the First Metatarsal in HAV the Result of First TMT Joint Rotation?
A distinct contributor to a pronated position of the first metatarsal is intrinsic “twist” or torsion in the shaft of the bone. Two studies using standard CT imaging showed approximately 12 degrees more eversion torsion in the first metatarsal in HAV patients compared to healthy controls.42,43 Another study using true weight-bearing CT imaging showed that patients with HAV have a significant 9 degrees greater eversion torsion in the first metatarsal compared to healthy subjects.44

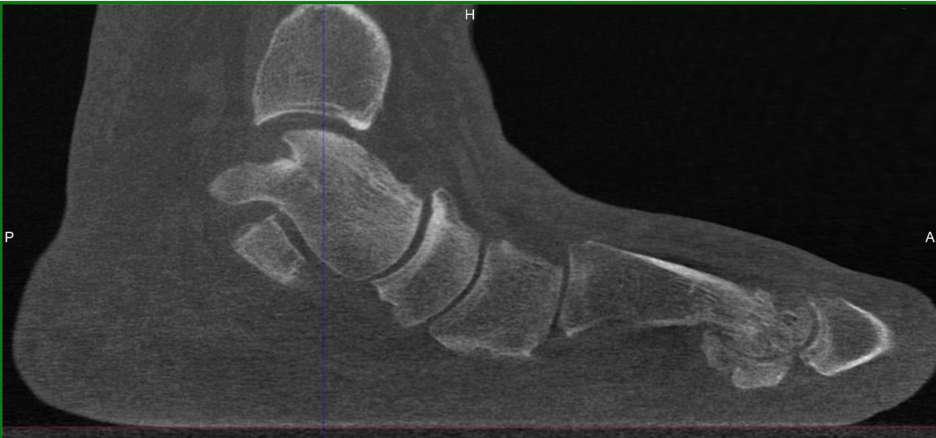
In terms of joint rotation, the first TMT joint moves in the direction of supination, not pronation in patient with HAV. Three studies using standard CT imaging compared joint positions of the medial column of the feet in both an unloaded and loaded condition. The studies compared these joint rotations in patients with HAV deformity and healthy control patients. Geng and colleagues observed that the first metatarsal moved in the direction of inversion, dorsiflexion and adduction relative to the medial cuneiform and the magnitude of this motion was greater in all 3 planes in the patients with HAV deformity.29 Watanabe found that both HAV patients and controls demonstrated equal magnitude of 5 degrees eversion of the navicular with loading of the foot, while the HAV patients demonstrated greater inversion (2 degrees) of the first metatarsal relative to the medial cuneiform than controls.45 There was minimal coronal plane rotation of the cuneiform in both groups. Kimura and colleagues found that the talonavicular joint rotated in the direction of eversion, with greater magnitude and variability in the HV group.46 At the first naviculocuneiform joint, the HAV patients showed eversion at a magnitude of only 0.2 degrees while control patients showed mild 1.5 degrees inversion. At the first TMT joint 4.9 degrees inversion occurred in the first metatarsal with loading of the foot. In addition, dorsal hypermobility of the first ray was present in patients with HAV deformity who exhibited more dorsiflexion at the first TMT joint than healthy controls. The overall net frontal plane motion of the medial column was in the direction of eversion, primarily due to motion of the navicular on the talus. Pronation motion of the navicular measured 9.6 degrees, which offset 4.9 degrees of supination motion of the first metatarsal at the first TMT joint. Therefore, when the entire foot pronates, the net pronation or eversion of the joints proximal to the first TMT articulation can ultimately place the first metatarsal everted to the ground (Figures 2A-E).
It is clear that the center of pronation rotation of the medial column of the foot in HAV patients is the talonavicular joint, not the first TMT joint. In the 3 studies of joint motion in HAV patients, the first TMT always moved in the direction of supination with loading of the foot.29,45,46
Does a Pre-Existing Deformity in the first TMT Joint Cause Metatarsus Primus Varus?
Several factors can result in greater adduction positioning of the first TMT joint. Instability can be the result of ligamentous laxity, abnormal angulation of the medial cuneiform joint surface, or variation in morphology of the joint surface allowing greater joint mobility.
Mobility of the first TMT joint in the transverse plane is required for the development of metatarsus primus varus as well as a progressive increase of the hallux valgus angular deformity. Whether hypermobility of the first TMT joint in the transverse plane is the primary etiology of HAV deformity has yet to be proven. Kimura and colleagues identified greater adduction motion of the first TMT joint in HAV patients compared to healthy controls (3.2 degrees vs 1.1 degree).46 In another study Kimura and colleagues measured greater mobility in the medial and second intercuneiform joint in HAV patients compared to controls, suggesting that transverse plane instability can emanate from this articulation as well as the first TMT joint.47 Kimura and colleagues were unable to determine if the greater inter-cuneiform joint mobility they measured was the result versus the cause of HAV deformity.
Faber and colleagues applied both a dorsal directed and medial directed force on the head of the first metatarsal in 9 cadaver specimens.48 Faber found the first TMT joint contributed 82% of the medial motion of the first ray joints, but could not find a correlation between the magnitude of displacement of the first metatarsal and degree of hallux valgus angle. Also, no correlation was found between first TMT joint angular displacement and the shape of the first TMT, the number of facets of the first TMT joint, and the existence of a joint between the first and second metatarsals.
Researchers have often cited medial inclination or obliquity of the articular surface of the medial cuneiform as a primary cause of progressive metatarsus primus varus.12,49-51 However, most studies of medial cuneiform obliquity used standing radiographs, which are unreliable as they are significantly affected by the angle of the radiographic beam or by foot positioning. Brage and colleagues found that a 10-degree radiographic beam angle will increase medial inclination of the medial cuneiform by 7.2 degrees compared to a 20-degree radiographic beam angle.52 Doty,53 Sanicola,54 and Khoury55 reported similar findings, and Khoury also showed that positioning of the foot and angulation of the first ray can significantly affect the appearance of obliquity of the distal articulation surface of the medial cuneiform.
A recent study by Li and colleagues implemented improved methodology using CT imaging and a 3D coordinate system to evaluate the morphology of the medial cuneiform, independent of positioning of the bone on the ground.56 In this study, there were no statistical differences found when comparing HAV patients and control patients in terms of medial cuneiform joint surface angulation or obliquity of the first TMT joint surface. However, an interesting finding from the study conducted by Li and colleagues was that patients with HAV showed a flatter joint surface at the distal medial cuneiform than healthy controls.
Other investigators have reported variations in the morphology of the articular surface or the configuration of joint cartilage of the first TMT joint. Hyer and colleagues studied the base of the first metatarsal bone in 77 specimens, denuded of all cartilage and soft tissue attachments.57 They reported that 22 of 77 (29%) first metatarsals had evidence of an intermetatarsal facet, which was associated with an increase in the medial inclination angle of the first TMT joint. A cadaver study conducted by Mason and Tanaka found that only specimens with HAV had a single-facet configuration of the first TMT joint while normal specimens had a 3-facet morphology.58 Doty and colleagues found that feet with a flatter, continuous articular surface at the base of the first metatarsal had a higher intermetatarsal angle (12.1 degrees) than feet with a bilobed articular surface (9.7 degrees).47
A recent weight-bearing CT study gives even more intriguing evidence of distinct morphology of the first TMT joint, which may contribute to HAV deformity. Ji and colleagues studied 82 feet with hallux valgus and compared to 79 healthy feet.59 A flatter inferior lateral facet and wider middle facet width on the articular surface of the base of the first metatarsal was clearly associated with more severe parameters of hallux valgus. The continuous flat type of articular surface was associated with a higher intermetatarsal angle and showed greater plantar gapping at the first TMT joint compared with the separated-protruded type of cartilage. Most intriguing was the presence of a continuous-flat type of facet in 74.4% of the HAV group compared to only 16.5% of the control group. The control group was more likely to have a 3-facet type of cartilage on the articular surface (481%) compared to the HAV group (7.3%). The authors proposed that a flatter joint surface has reduced interlocking and greater joint mobility as evidenced in previous studies.60,61
These morphologic features of the first TMT joint described in multiple studies are not the root cause of a bunion as they are not present in all feet with HAV deformity. However, just like a pronated position of the first metatarsal, morphologic features of the articular surfaces of the first TMT joint may be a risk factor which, combined with other known risk factors, may initiate progressive HAV deformity.
Variations in the morphology of the joint surfaces of the first TMT joint cannot create instability unless a force acts upon that joint. Ground reaction forces as well as moment generated by muscles acting across multiple joints of the first ray may affect the first TMT differently depending upon joint morphology. This illustrates why and how multiple factors come into play in the pathogenesis of HAV deformity as verified by multiple investigations.

Excessive pronation of the talonavicular joint may position the head of the first metatarsal on the ground in an everted position.46 Ground reaction forces are then directed medially against the sesamoid apparatus creating strain on the medial collateral ligaments of the first metatarsophalangeal joint.39,40 When the head of the first metatarsal escapes medially from the stabilizing soft tissue envelope surrounding the sesamoid apparatus, dorsal instability of the first ray ensues.20,23 Attrition of the medial collateral ligaments of the first metatarsophalangeal joint may occur due to inherited genetic variants causing aberration in collagen structure.62,63 When the hallux is pushed laterally by restrictive footwear, retrograde force generated by the flexor hallucis longus and brevis muscles creates adduction moment proximally on the first TMT joint (Figure 3).64-68 If a patient has congenital weakness of the abductor hallucis muscle, the adductor hallucis is unopposed causing a similar retrograde adduction torque on the first TMT joint.69-71 Individuals may have certain morphology of the articular surfaces of the first TMT joint, which can resist these abnormal forces while other people may have distinct features which will allow this joint to gradually shift alignment over time. Certainly, multiple factors must come into play acting at locations proximal and distal to the first TMT joint.
Summary
Hallux abductovalgus is a triplane deformity that results from instability at multiple joints in the medial column of the foot. Pronation rotation of the first metatarsal originates at the talonavicular joint. Sagittal plane and transverse plane instability of the first TMT joint can be a secondary change when there is loss of alignment of soft tissue structures located distally around the first MTPJ. Recent research has verified that certain unique features in the shape and configuration of the articular surfaces of the first TMT may cause instability in the transverse and sagittal planes. These unique anatomic features may render the first TMT vulnerable to torque from malalignment the first MTPJ or may directly cause instability at the first TMT leading to the development of HAV deformity.
Dr. Richie is an Associate Clinical Professor at California School of Podiatric Medicine at Samuel Merritt University.
References
1. Dayton P, Feilmeier M, Kauwe M, Hirschi J. Relationship of frontal plane rotation of first metatarsal to proximal articular set angle and hallux alignment in patients undergoing tarsometatarsal arthrodesis for hallux abducto valgus: a case series and critical review of the literature. J Foot Ankle Surg. 2013;52(3):348-354.
2. Dayton P, Kauwe M, Feilmeier M. Is our current paradigm for evaluation and management of the bunion deformity flawed? A discussion of procedure philosophy relative to anatomy. J Foot Ankle Surg. 2015;54(1):102-11.
3. Paley D, Herzenber JE. Principles of Deformity Correction. Springer-Verlag, Berlin, 2005.
4. Wagner E, Ortiz C, Wagner P. Using the center of rotation of angulation concept in hallux valgus correction: why do we choose the proximal oblique sliding closing wedge osteotomy? Foot Ankle Clin. 2018;23(2):247-256.
5. Mashima N, Yamamoto H, Tsuboi I, Tsuchiya H, Tanaka Y, Watanabe S. Correction of hallux valgus deformity using the center of rotation of angulation method. J Orthop Sci. 2009;14(4):377-384.
6. Grode SE, McCarthy DJ. The anatomical implications of hallux abducto valgus: a cryomicrotomy study. J Am Podiatry Assoc. 1980;70:539–551.
7. Scranton PE Jr, Rutkowski R. Anatomic variations in the first ray: part I. Anatomic aspects related to bunion surgery. Clin Orthop Relat Res. 1980;151:244–255.
8. Mortier J-P, Bernard J-L, Maestro M. Axial rotation of the first metatarsal head in a normal population and hallux valgus patients. Orthop Traumatol Surg Res. 2012;98:677–683.
9. Kim Y, Kim JS, Young KW, Naraghi R, Cho HK, Lee SY. A new measure of tibial sesamoid position in hallux valgus in relation to the coronal rotation of the first metatarsal in CT scans. Foot Ankle Int. 2015;36:944–952.
10. Hatch DJ, Santrock RD, Smith B, Dayton P, Weil L Jr. Triplane hallux abducto valgus classification. J Foot Ankle Surg. 2018;57(5):972-981.
11. Klaue K, Hansen ST, Masquelet AC. Clinical, quantitative assessment of first tarsometatarsal mobility in the sagittal plane and its relation to hallux valgus deformity. Foot Ankle Int. 1994;15(1):9–13
12. Lapidus PW. Operative correction of metatarsus varus primus in hallux valgus. Surg Gynecol Obstet. 1934;58:183–191
13. Lee KT, Young K. Measurement of first-ray mobility in normal vs. hallux valgus patients. Foot Ankle Int. 2001;22(12):960–964.
14. Hansen ST Jr. Hallux valgus surgery. Morton and Lapidus were right! Clin Podiatr Med Surg. 1996;13(3):347–354.
15. Meyr AJ, Berkelbach C, Dreikorn C, Arean T. Descriptive quantitative analysis of first metatarsal sagittal plane motion. J Foot Ankle Surg. 2020;59(6):1244–1247.
16. Shibuya N, Roukis T, Jupiter DC. Mobility of the first ray in patients with or without hallux valgus deformity: Systematic review and meta-analysis. J Foot Ankle Surg. 2017;56(5):1070–1075.
17. Allen MK, Cuddeford TJ, Glasoe WM, et al. Relationship between static mobility of the first ray and first ray, midfoot, and hindfoot motion during gait. Foot Ankle Int. 2004;25(6):391–396.
18. Coughlin MJ, Jones CP. Hallux valgus and first ray mobility. A prospective study. J Bone Joint Surg Am. 2007;89(9):1887–1898.
19. Coughlin MJ, Jones CP, Viladot R, et al. Hallux valgus and first ray mobility: a cadaveric study. Foot Ankle Int. 2004;25(8):537–544
20. Coughlin MJ, Shurnas PS. Hallux valgus in men. Part II: first ray mobility after bunionectomy and factors associated with hallux valgus deformity. Foot Ankle Int. 2003;24(1):73–78
21. Kim JY, Park JS, Hwang SK, Young KW, Sung IH. Mobility changes of the first ray after hallux valgus surgery: clinical results after proximal metatarsal chevron osteotomy and distal soft tissue procedure. Foot Ankle Int. 2008;29(5):468–472.
22. Rush SM, Christensen JC, Johnson CH. Biomechanics of the first ray. Part II: metatarsus primus varus as a cause of hypermobility. A three-dimensional kinematic analysis in a cadaver model. J Foot Ankle Surg. 2000;39(2):68–77
23. Doty JF, Coughlin MJ. Hallux valgus and hypermobility of the first ray: facts and fiction. Int Orthop. 2013;37:1655–1660
24. Sharkey NA, Donahue SW, Ferris L. Biomechanical consequences of plantar fascial release or rupture during gait - Part II: Alterations in forefoot loading. Foot Ankle Int. 1999;20(2):86-96.
25. Kirane YM, Michelson JD, Sharkey NA. Contribution of the flexor hallucis longus to loading of the first metatarsal and first metatarsophalangeal joint. Foot Ankle Int. 2008;29(4):123-134.
26. Sharkey NA, Ferris L, Smith TS, et al. Strain and loading of the second metatarsal during heel-lift. J Bone Joint Surg Am. 1995;77(7):1050–1057.
27. Rush SM, Christensen JC, Johnson CH. Biomechanics of the first ray. Part 2: Metatarsus primus varus as a cause of hyper- mobility. A three-dimensional kinematic analysis in a cadaver model. J Foot Ankle Surg. 2000;39(2):68-77.
28. King DM, Toolan BC. Associated deformities and hypermobility in hallux valgus: an investigation with weightbearing radiographs. Foot Ankle Int. 2004;25:251–255.
29. Geng X, Wang C, Ma X, et al. Mobility of the first metatarsal-cuneiform joint in patients with and without hallux valgus: in vivo three-dimensional analysis using computerized tomography scan. J Orthop Surg Res. 2015;10:1–7
30. Lee HY, Lalevee M, Mansur NSB, et al. Multiplanar instability of the first tarsometatarsal joint in hallux valgus and hallux rigidus patients: a case-control study. Int Orthop. 2022;46(2):255-263.
31. Tashiro T, Ikuta Y, Maeda N, et al. First tarsometatarsal joint mobility in hallux valgus during gait: A synchronized ultrasound and three-dimensional motion capture analysis. J Med Ultrason. 2024;51(2):331-339.
32. Saltzman CL, Brandser EA, Anderson CM, Berbaum KS, Brown TD. Coronal plane rotation of the first metatarsal. Foot Ankle Int. 1996;17(3):157-161
33. Campbell B, Miller MC, Williams L, et al. Pilot study of a 3-dimensional method for analysis of pronation of the first metatarsal of hallux valgus patients. Foot Ankle Int. 2018;39(12):1449-1456.
34. Collan L, Kankare JA, Mattila K. The biomechanics of the first metatarsal bone in hallux valgus: a preliminary study utilizing a weight bearing extremity CT. Foot Ankle Surg. 2013;19(3):155-161.
35. Scheele CB, Christel ST, Fröhlich I, et al. A cone beam CT based 3D-assessment of bony forefoot geometry after modified Lapidus arthrodesis. Foot Ankle Surg. 2020;26(8):883-889.
36. Steadman J, Bakshi N, Arena C, Leake R, Barg A, Saltzman C. Normative distribution of first metatarsal axial rotation. Foot Ankle Int. 2021;42(8):1040–1048.
37. Najefi A, Zaveri A, Alsafi MK, Malhotra K, Patel S, Cullen N, Welck M. The assessment of first metatarsal rotation in the normal adult population using weight bearing computed tomography. Foot Ankle Int. 2021; 42(10):1223–1230
38. Mahmoud K, Metikala S, Mehta SD, Fryhofer GW, Farber DC, Prat D. The role of weightbearing computed tomography scan in hallux valgus. Foot Ankle Int. 2021; 42:287–293.
39. Lalevée M, de Carvalho KAM, Barbachan Mansur NS, et al. Distribution, prevalence, and impact on the metatarsosesamoid complex of first metatarsal pronation in hallux valgus. Foot Ankle Surg. 2023 Aug;29(6):488-496. doi: 10.1016/j.fas.2023.06.003.
40. Lalevée M, Dibbern K, Barbachan Mansur NS, et al. Impact of first metatarsal hyperpronation on first ray alignment: a study in cadavers. Clin Orthop Relat Res. 2022; 480(10):2029-2040.
41. Okuda R, Kinoshita M, Yasuda T, Jotoku T, Kitano N, Shima H. The shape of the lateral edge of the first metatarsal head as a risk factor for recurrence of hallux valgus. J Bone Joint Surg Am. 2007;89(10):2163-2172.
42. Ota T, Nagura T, Kokubo T, et al. Etiological factors in hallux valgus, a three-dimensional analysis of the first metatarsal. J Foot Ankle Res. 2017;10(43):1–6. doi:10.1186/s13047-017-0226-1
43. Cruz EP, Wagner FV, Henning C, et al. Does hallux valgus exhibit a deformity inherent to the first metatarsal bone? J Foot Ankle Surg. 2019;58(6):1210-1214. doi:10.1053/j.jfas.2018.09.031
44. Randich JR, John JK, Gomez K, et al. Frontal plane rotation of the first ray in hallux valgus using standing computerized tomography (CT). J Foot Ankle Surg. 2021; 60(3):489-493. doi:10.1053/j.jfas.2020.05.022
45. Watanabe K, Ikeda Y, Suzuki D, et al. Three-dimensional analysis of tarsal bone response to axial loading in patients with hallux valgus and normal feet. Clin Biomech. 2017;42:65–69. doi:10.1016/j.clinbiomech.2017.01.012
46.Kimura T, Kubota M, Taguchi T, et al. Evaluation of first-ray mobility in patients with hallux valgus using weight-bearing CT and a 3-D analysis system: a comparison with normal feet. JBJS. 2017;99(3):247-255. doi:10.2106/JBJS.16.00542
47. Kimura T, Kubota M, Suzuki N, Hattori A, Marumo K. Comparison of Intercuneiform 1-2 joint mobility between hallux valgus and normal feet using weightbearing computed tomography and 3-dimensional analysis. Foot Ankle Int. 2018 Mar;39(3):355-360. doi: 10.1177/1071100717744174. Epub 2017 Dec 4. PMID: 29198142.
48. Faber FW, Kleinrensink GJ, Verhoog MW, et al. Mobility of the first tarsometatarsal joint in relation to hallux valgus deformity: anatomical and biomechanical aspects. Foot Ankle Int. 1999; 20:651–656.
49. Golano P, Viladot R, Alvarez F, Coughlin M, Grimes JS. Static loading of foot structures for radiographic studies. Foot Ankle Int. 2006;27:559-560.
50. Vyas S, Conduah A, Vyas N, Otsuka NY. The role of the first metarsocuneiform joint in juvenile hallux valgus. J Pediatr Orthop B. 2010; 19:399–402. https:// doi. org/ 10. 1097/ BPB. 0b013 e3283 3af4dc
51. Bu P, Li C, Pu L et al. Radiographic assessment of relationship between medial cuneiform obliquity and hallux valgus. J Foot Ankle Surg. 2023; 62(3):583-89. https:// doi. org/ 10. 1053/j. jfas. 2022. 06. 009
52. Brage ME, Holmes JR, Sangeorzan BJ. The influence of X-ray orientation on the first metatarsocuneiform joint angle. Foot Ankle Int. 1994; 15(9):495–497. https:// doi. org/ 10. 1177/ 10711 00794 01500 907
53. Doty JF, Coughlin MJ, Hirose C, et al. First metatarsocuneiform joint mobility: radiographic, anatomic, and clinical characteristics of the articular surface. Foot Ankle Int. 2014 May;35(5):504-11. doi: 10.1177/1071100714524556. Epub 2014 Feb 21. PMID: 24563392.
54. Sanicola SM, Arnold TB, Osher L. Is the radiographic appearance of the hallucal tarsometatarsal joint representative of its true anatomical structure? J Am Podiatr Med Assoc. 2002; 92:491–498.https:// doi. org/ 10. 7547/ 87507 315- 92-9- 491
55. Koury K, Staggers JR, Pinto MC, et al. Radiographic assessment of first tarsometatarsal joint shape and orientation. Foot Ankle Int. 2019; 40:1438–1446. https:// doi. org/ 10. 1177/ 10711 00719 868503
56. Li R, Tan K, Xie Y, Wang F. Morphology variations with medial cuneiform in hallux valgus. Anat Sci Int. 2024 Jan;99(1):59-67. doi: 10.1007/s12565-023-00734-6. Epub 2023 Jul 15. PMID: 37453991.
57. Hyer CF, Philbin TM, Berlet GC, Lee TH. The incidence of the intermetatarsal facet of the first metatarsal and its relationship to metatarsus primus varus: a cadaveric study. J Foot Ankle Surg. 2005 May-Jun;44(3):200-2. doi: 10.1053/j.jfas.2005.03.001. PMID: 15940598.
58. Mason LW, Tanaka H. The first tarsometatarsal joint and its association with hallux valgus. Bone Joint Res. 2012;1(6):99- 103
59. Ji L, Ding S, Zhang M, Colon Reyes K, Zhu M, Sun C. The role of first tarsometatarsal joint morphology and instability in the etiology of hallux valgus: a case-control study. Foot Ankle Int. 2023 Aug;44(8):778-787. doi: 10.1177/10711007231175846. Epub 2023 Jul 1. PMID: 37392055.
60. Dykyj D, Ateshian GA, Trepal MJ, MacDonald LR. Articular geometry of the medial tarsometatarsal joint in the foot: comparison of metatarsus primus adductus and metatarsus primus rectus. J Foot Ankle Surg. 2001; 40(6):357–365.
61. Nozaki S, Watanabe K, Kamiya T, et al. Sex- and age-related morphological variations in the talar articular surfaces of the calcaneus. Ann Anat Anat Anz. 2020; 229:151468.
62.Uchiyama E, Kitaoka HB, Luo ZP, Grande JP, Kura H, An KN. Pathomechanics of hallux valgus: biomechanical and immunohistochemical study. Foot Ankle Int. 2005; 26(9):732-8.
63. Arbeeva L, Yau M, Mitchell BD, et al. Genome-wide meta-analysis identified novel variant associated with hallux valgus in Caucasians. J Foot Ankle Res. 2020 Mar 4;13(1):11. doi: 10.1186/s13047-020-0379-1. PMID: 32131869; PMCID: PMC7057609.
64. Nix SE, Vicenzino BT, Collins NJ, Smith MD. Characteristics of foot structure and footwear associated with hallux valgus: a systematic review. Osteoarthritis Cartilage. 2012;20(10):1059–1074.
65. Shine IB. Incidence of hallux valgus in a partially shoe-wearing community. Brit Med Jour. 1965; 7(1):1648-1650.
66. Menz HB, Roddy E, Marshall M, et al. Epidemiology of shoe wearing patterns over time in older women: associations with foot pain and hallux valgus. J Gerontol A Biol Sci Med Sci. 2016;71(12):1682–7.
67. Klein C, Groll-Knapp E, Kundi M, Kinz W. Increased hallux angle in children and its association with insufficient length of footwear: A community based cross-sectional study. BMC Musculoskelet Disord. 2009; 17:159.
68. Snijders CJ, Snijder JG, Philippens MM. Biomechanics of hallux valgus and spread foot. Foot Ankle. 1986;7(1):26-39.
69. Mortka K, Lisiński P, Wiertel-Krawczuk A. The study of surface electromyography used for the assessment of abductor hallucis muscle activity in patients with hallux valgus. Physiother Theory Pract. 2018;34(11):846-851. doi:10.1080/09593985.2018.1430879
70. Arinci Incel N, Genç H, Erdem HR, Yorgancioglu ZR. Muscle imbalance in hallux valgus: an electromyographic study. Am J Phys Med Rehabil. 2003;82(5):345-349. doi:10.1097/01.PHM.0000064718.24109.26
71. Stewart S, Ellis R, Heath M, Rome K. Ultrasonic evaluation of the abductor hallucis muscle in hallux valgus: A cross-sectional observational study. BioMed Central Musculoskeletal Disorders. 2013; 14:45











