Addressing Complications Of Retained Foreign Bodies
Retained foreign bodies are a relatively common injury and over 50 percent of foreign body injuries affect the foot.1,2 The most common foreign bodies are needles, metal, glass, wood, plastic and stone. Due to potential complications from retained foreign bodies, one should remove them unless removal puts neurovascular or other critical structures at high risk of iatrogenic damage. Possible complications from retained foreign bodies include infection, migration, stiffness, granuloma formation and pain. Pain and stiffness. Both the type and location of a foreign body will influence the amount of resulting pain and stiffness. Foreign bodies located within tendons, tendon sheaths and near joints frequently result in joint pain and stiffness. Reactive inflammation, which researchers have found to be greatest with organic material, is also a significant cause of pain.3 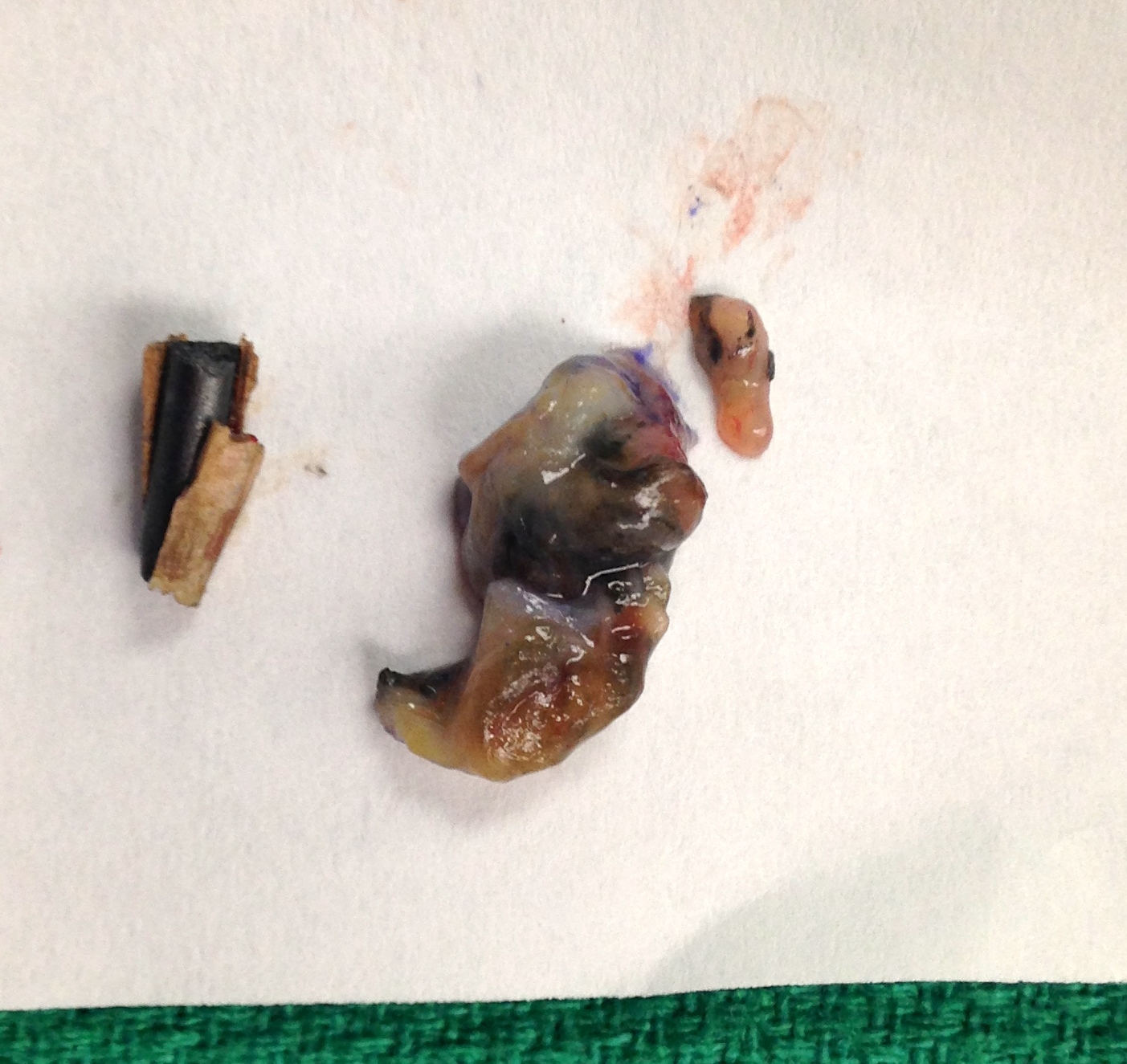 Authors have reported other rare foreign body complications leading to pain and stiffness. Dar and colleagues report a case of third toe contracture due to plantar fascial fibrosis secondary to a retained rubber foreign body in the foot.4 Nerve compression secondary to foreign bodies and foreign body granuloma formation is another rare cause of pain. Kurtulmus and coworkers report the formation of foreign body granuloma and nerve compression with resultant carpal tunnel syndrome following a retained stone in the hand.1 Infection. Studies have reported infection rates raging from 1.1 to 12 percent secondary to retained foreign bodies.5 Several factors affect the risk of infection secondary to a foreign body including the time since the initial injury, the type of foreign body, wound contamination and the patient's health status. Hollander and colleagues found that older patients and patients with diabetes are at a higher risk of infection from retained foreign bodies.6 Wound contamination was also associated with increased risk of infection. Due to their organic nature, wood foreign bodies cause the highest risk of infection and inflammation.7 Even though infection remains the most common complication of foreign bodies, authors do not recommend routine antibiotic prophylaxis.5 Although rare, tetanus is also a risk following a significant puncture wound or the retention of a foreign body. One should thoroughly review the tetanus status of all patients with a puncture wound or retained foreign body. Patients should receive prophylactic tetanus toxoid and tetanus immune globulin if they have not had tetanus immunization within 10 years and there is wound contamination.8 Migration. Migration of foreign bodies is another potential complication. Both the properties of the foreign body and its anatomic location influence foreign body migration. Long, thin, smooth foreign bodies located in tendon sheaths and the upper extremities tend to move more easily and over longer distances.1,9-11 The fibrous septa of the plantar fat pad restricts foreign body migration in the plantar foot.9 Foreign body granuloma. A foreign body granuloma is an inflammatory, histolytic and macrophage tissue reaction pattern that occurs in response to exogenous material that penetrates the dermis. Histologically, the lesions are characterized by a predominantly multinucleated giant cell infiltrate that also contains histiocytes, lymphocytes and other inflammatory cells.12 Foreign body granulomas can present as pseudotumors of both bone and soft tissue, often years after the initial injury. Vega and colleagues reported several cases of foreign body granuloma, pseudo-tumor formation and bone changes secondary to retained foreign bodies.13 Bouchti and Durr and their respective co-workers report cases of thorns inducing lytic lesions of the metatarsals.14-15
Authors have reported other rare foreign body complications leading to pain and stiffness. Dar and colleagues report a case of third toe contracture due to plantar fascial fibrosis secondary to a retained rubber foreign body in the foot.4 Nerve compression secondary to foreign bodies and foreign body granuloma formation is another rare cause of pain. Kurtulmus and coworkers report the formation of foreign body granuloma and nerve compression with resultant carpal tunnel syndrome following a retained stone in the hand.1 Infection. Studies have reported infection rates raging from 1.1 to 12 percent secondary to retained foreign bodies.5 Several factors affect the risk of infection secondary to a foreign body including the time since the initial injury, the type of foreign body, wound contamination and the patient's health status. Hollander and colleagues found that older patients and patients with diabetes are at a higher risk of infection from retained foreign bodies.6 Wound contamination was also associated with increased risk of infection. Due to their organic nature, wood foreign bodies cause the highest risk of infection and inflammation.7 Even though infection remains the most common complication of foreign bodies, authors do not recommend routine antibiotic prophylaxis.5 Although rare, tetanus is also a risk following a significant puncture wound or the retention of a foreign body. One should thoroughly review the tetanus status of all patients with a puncture wound or retained foreign body. Patients should receive prophylactic tetanus toxoid and tetanus immune globulin if they have not had tetanus immunization within 10 years and there is wound contamination.8 Migration. Migration of foreign bodies is another potential complication. Both the properties of the foreign body and its anatomic location influence foreign body migration. Long, thin, smooth foreign bodies located in tendon sheaths and the upper extremities tend to move more easily and over longer distances.1,9-11 The fibrous septa of the plantar fat pad restricts foreign body migration in the plantar foot.9 Foreign body granuloma. A foreign body granuloma is an inflammatory, histolytic and macrophage tissue reaction pattern that occurs in response to exogenous material that penetrates the dermis. Histologically, the lesions are characterized by a predominantly multinucleated giant cell infiltrate that also contains histiocytes, lymphocytes and other inflammatory cells.12 Foreign body granulomas can present as pseudotumors of both bone and soft tissue, often years after the initial injury. Vega and colleagues reported several cases of foreign body granuloma, pseudo-tumor formation and bone changes secondary to retained foreign bodies.13 Bouchti and Durr and their respective co-workers report cases of thorns inducing lytic lesions of the metatarsals.14-15
In Conclusion
Potential complications from retained foreign bodies include infection, migration, stiffness, granuloma formation and pain. Infection remains the most common complication of foreign bodies but authors do not recommend routine antibiotic prophylaxis.5 Organic foreign bodies, most commonly wood, have the highest potential to cause pain, inflammation and infection. Given the potential complications from foreign bodies, remove them unless there is substantial risk from the procedure.1,2 References 1. Kurtulmus T, Saglam N, Saka G, Imam M, Akpinar F. Tips and tricks in the diagnostic workup and removal of foreign bodies in extremities. Acta Orthop Traumatol Turc. 2013;47(3):387-392. 2. Nagendran T. Management of foreign bodies in the emergency department. Hospital Physician. 1999;35(9):27-40. 3. Lammers RL. Soft tissue foreign bodies. Ann Emerg Med. 1988;17(12):13368;17 4. Dar TA, Sultan A, Hussain S, Dhar SA, Ali MF. Contracture of the third toe as a delayed presentation of a foreign body in the foot. Foot Ankle Spec. 2011;4(5):298-300. 5. Cummings P, Del Beccaro MA. Antibiotics to prevent infection of simple wounds: a meta-analysis of randomized studies. Am J Emerg Med. 1995;13(4):39695;13 6. Hollander JE, Singer AJ, Valentine SM, Shofer FS. Risk factors for infection in patients with traumatic lacerations. Acad Emerg Med. 2001;8(7):716-20. 7. Lammers RL, Magill T. Detection and management of foreign bodies in soft tissue. Emerg Med Clin North Am. 1992;10(4):76792;1 8. Halaas GW. Management of foreign bodies in the skin. Am Fam Physician. 2007;76(5):683-8. 9. Vargas B, Wildhaber B, La Scala G. Late migration of a foreign body in the foot 5 years after initial trauma. Pediatr Emerg Care. 2011;27(6):535-6. 10. Gregory B, Anvesh R, Moroz PJ. Foreign body migration along a tendon sheath in the lower extremity: a case report and literature review. J Bone Joint Surg Am. 2011; 93(8):e38. 11. Bu J, Overgaard KA, Viegas SF. Distal migration of a foreign body (sago palm thorn fragment) within the long-finger flexor tendon sheath. Am J Orthop. 2008;37(4):208-209. 12. Weedon D. Foreign Body Granulomas. In Weddon's Skin Pathology Third Edition, Chapter 7, Elsevier, London, 2010. 13. Vega CA, Villaverde RM, Carrillo LF, Bermudo RP, Bencano C. Injuries from palm tree simulating tumoral or pseudotumoral bone lesions. Acta Orthop Belg. 2001; 67(3):279-82. 14. Durr HR, Stäbler A, Müller PE, Refior HJ. Thorn-induced pseudotumor of the metatarsal: a case report. J Bone Joint Surg. 2001;83(4):585. 15. Bouchti IE, Essi FA, Abkari I, Hassani SE. Foreign body granuloma: a diagnosis not to forget. Case Rep Orthop. 2012;2012:439836. doi: 10.1155/2012/439836. Epub 2012 Mar 26.











