Complex High Risk Percutaneous Coronary Intervention in a 54-Year-Old Patient After Surgical Turndown and a Unique Approach to the Heart Team
© 2025 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Cath Lab Digest or HMP Global, their employees, and affiliates.
Aaron Ali Shaikh, MD1; Bernardo Cortese, MD, FESC, FSCAI2
1CHIP-CTO Fellow, University Hospitals; 2Interventional Director of the Coronary Center, University Hospitals Harrington Heart & Vascular Institute, University Hospitals Cleveland Medical Center, Cleveland, Ohio
Dr. Cortese can be contacted at bernardo.cortese@uhhospitals.org
Read more in an interview with operator Bernardo Cortese, MD, FESC, FSCAI.
Patient Presentation
A 54-year-old male with a past medical history of Hodgkin’s lymphoma with previous chemo and radiation therapy 22 years ago and type II diabetes initially presented at an outlying hospital with acute onset dyspnea. An initial electrocardiogram demonstrated atrial fibrillation with rapid ventricular response. He developed hemodynamic instability and was emergently cardioverted to normal sinus rhythm. High-sensitivity troponin was elevated to 300 ng/L and trended upwards to >25,000 ng/L. He was admitted to intensive care unit, and redeveloped atrial fibrillation with rapid ventricular response and further hemodynamic instability that degraded to cardiac arrest with pulseless electrical activity. He received 3 minutes of cardiopulmonary resuscitation with spontaneous return of circulation and was initiated on mechanical ventilation, regaining consciousness shortly thereafter. A transthoracic echocardiogram demonstrated reduced left ventricular systolic function with apical hypokinesis.
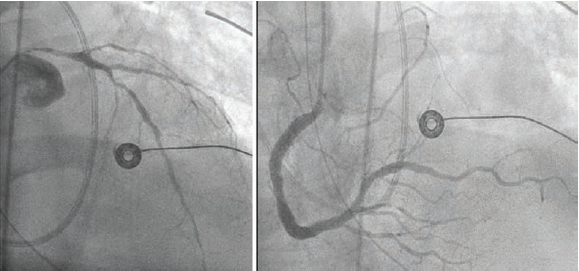
At the outlying hospital, the patient underwent invasive coronary angiography that demonstrated severe multivessel coronary artery disease involving the entire left main coronary artery, severe diffuse disease in the left anterior descending artery (LAD), and a chronic total occlusion of the circumflex artery with right-to-left collateral flow from the distal right coronary artery that had mild-moderate stenosis in the mid segment. An intra-aortic balloon pump (IABP) was implanted via right common femoral access (Figure 1).

The patient was initially referred for transfer to the tertiary care center of the outlying hospital’s healthcare system, but due to logistics, his transfer was significantly delayed. He was then promptly transferred to our tertiary care center, University Hospitals Harrington Heart & Vascular Institute at University Hospitals Cleveland Medical Center, for cardiac surgery consultation. He was extubated shortly after transfer.
A multidisciplinary heart team discussion was performed immediately online on that Sunday morning. It included the cardiovascular intensive care unit (CICU) attending, the cardiac surgeon, and our team of interventional cardiology, and resulted in the decision of urgent percutaneous revascularization of the left main coronary artery and LAD under IABP assistance because cardiac surgery was refused due to previous radiotherapy. This plan was discussed with the patient who had excellent neurologic recovery and he gave his consent to undergo high-risk percutaneous coronary intervention (PCI).

proximal refence diameter in the LMCA (right).
Case
A 6 French right radial access was obtained and the left main coronary artery (LMCA) was cannulated. The first diagonal branch was wired and the LAD was wired with a second wire. Pre-dilation from the mid LAD back into the LMCA was performed with 2.0 x 20 mm semicompliant balloon. Intravascular ultrasound (IVUS) was then performed with the Refinity short-tip rotational IVUS catheter (Philips) in the mid LAD into the LMCA, and demonstrated fibrocalcific plaque with segments of circumferential calcium (Figure 2). The distal reference diameter was measured as 3.4 mm in the LAD and proximal reference diameter as 4.2 mm in the LMCA (Figure 3).

calcium fracture.
Given the fibrocalcific disease visualized on IVUS, we performed plaque modification with a 3.5 x 15 mm Wolverine cutting balloon (Boston Scientific) with several inflations from the mid LAD to the ostium of the LMCA. IVUS re-assessment demonstrated calcium fracture, indicating the lesion was adequately prepared to accommodate a stent (Figure 4).

We then deployed a 4.0 mm x 24 mm Synergy Megatron stent (Boston Scientific) covering the ostium of the LMCA to the proximal LAD. The mid LAD was treated with 2.75 mm x 15 mm Resolute Onyx stent (Medtronic) deployed just distal to the take-off of the first diagonal branch, with a good final result (Figure 5). Post-stent IVUS demonstrated a minimal stent area of 5.4 mm2 within the mid-LAD stent and 13.7 mm2 within the LMCA (Figure 6).

The IABP was removed the following day. The patient was discharged to home post-op day 2 on triple therapy with apixaban in the setting of new-onset atrial fibrillation during the initial presentation. He was seen in the outpatient clinic approximately two months after discharge and was asymptomatic with no clinical evidence of heart failure. Aspirin was discontinued.
Discussion
This case highlights the effective utilization of the heart team approach at our institution. At University Hospitals Harrington Heart & Vascular Institute’s Coronary Center, we schedule weekly heart team discussions, during which patients with complex coronary anatomy and clinical presentation are discussed within a multidisciplinary group of interventional cardiologists, general cardiologists, and cardiac surgeons. The goal of these discussion is to arrive at a plan — whether surgical, percutaneous, or medical — that is tailored to the individual patient. We longitudinally follow these patients and log their clinical outcomes. A heart team meeting can be at any time of the week due to the need for urgent consultation, because we realized that some patients arrive to our tertiary center with a need for acute intervention. We reserve time each day for the heart team to discuss these acute cases on an “as-needed” basis in order to provide efficient and effective care. We term this the Rapid Multidisciplinary Discussion (RMD). The case presented herein was refused by another healthcare system and arrived at our institution on a Sunday morning. It was presented to the RMD that same day and the patient immediately received an imaging-based, high-risk PCI. This efficient delivery of care was the result of nimbleness of our Coronary Center’s approach to the heart team via our unique RMD framework.
Read more in an interview with operator Bernardo Cortese, MD, FESC, FSCAI.










